Office of Research & Development |
 |
Office of Research & Development |
 |

VA Research Currents archive
February 28, 2014

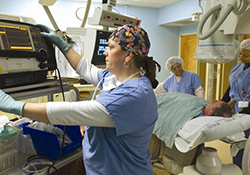
Research shows Veterans who were exposed to the intense stress of combat may be at higher risk for heart disease and other physical health problems later in life, regardless of whether they ever developed full-blown PTSD. (Photo by Staff Sgt. Staci Miller)
Science is catching up with what many war Veterans have long sensed: Emotional trauma isn't about only the mind. It also affects the body—especially the heart.
"There's now a large body of evidence that unequivocally links trauma exposure to poor physical health," says Dr. Paula Schnurr of VA's National Center for Posttraumatic Stress Disorder. She says an Israeli study published in 1989 was "one of the early studies suggesting PTSD was associated with impaired cardiovascular function." Fast-forward a quarter-century, and the literature backing that link is robust. Much of it has come from VA authors.
A 2013 article by VA and UCSD researchers even posed the provocative question of whether PTSD is a "fast track to premature cardiovascular disease."
Is there in fact the scientific equivalent of a smoking gun establishing a direct causal link between PTSD and heart disease? Not quite. But the research seems to be moving in that direction. Dr. Stephen Sidney, with Kaiser Permanente, wrote in a recent editorial in the Journal of the American College of Cardiology: "Overall, there are considerable data supporting an association that is likely causal between PTSD and coronary heart disease outcomes."
Still, plenty of questions remain: How exactly does PTSD play out in the cardiovascular system? Is it strictly a cause-and-effect relationship, or is the link more complex? Could there be pre-existing risk factors—say, gene variants—that raise someone's risk for both PTSD and heart disease? And how do poor health behaviors, such as smoking, and accompanying psychiatric conditions, such as depression, jumble the equation?
The answers are important for America's war Veterans. PTSD is estimated to affect between 11 and 20 percent of Afghanistan and Iraq Veterans. And VA cares for tens of thousands of Vietnam Veterans who are still coping with PTSD after four decades. About 3 in 10 Veterans from the Vietnam era have struggled with the condition.
PTSD by itself is a major health challenge. Higher rates of heart disease drive down quality of life even more—and drive up the risk of an earlier death. There are treatments for both conditions. But the better that doctors understand the nexus between them, the more they can focus on therapies likely to have a huge impact—and maybe prevent some problems from occurring in the first place. For example, if inflammation linked to PTSD turns out to be a key catalyst of heart disease, dietary changes could target that factor.
Just as important, hard proof of the impact of PTSD on cardiac health could be the extra push some Veterans need to seek mental health treatment.
"We can show Veterans there's an opportunity here. If we can work on reducing their PTSD symptoms, it could improve how they are feeling both mentally and physically," says Dr. Beth Cohen, an internist at the San Francisco VA Medical Center who studies the link between PTSD and heart health.
Cohen's group recently provided robust evidence of the PTSD-cardiac link, as part of their work on the Mind Your Heart Study. Published Dec. 1, 2013, in Biological Psychiatry, the study involved 663 Veterans at two VA sites in California. The patients walked on a treadmill while hooked up to an electrocardiogram, or EKG, which traces the heart's electrical activity as it pumps blood. Those who met the criteria for PTSD—about a third of the patients—were more likely to have EKGs showing reduced blood flow to the heart, or ischemia. The condition was present in 17 percent of the PTSD group, compared with 10 percent of the non-PTSD group.
After the researchers adjusted for clinical and demographic factors known to influence heart disease—age, past heart disease, C-reactive protein (a blood marker of inflammation), obesity, alcohol use, sleep quality, social support, depression—PTSD was associated with more than double the risk for ischemia.
Also, the more severe the PTSD symptoms, the greater the risk of ischemia. According to Sidney of Kaiser Permanente, being able to show such "dose response relationships" bolsters the theory that PTSD does lead to heart disease. Also critical in this regard, he says, are studies that shed light on plausible biological mechanisms that might explain the relationships.
One strength of Cohen's treadmill study was that it used objective measures of PTSD and heart disease, rather than patients' own accounts of their symptoms.
"Self-report studies are important, and have guided much of the work we are doing today," says Cohen. "But finding strong associations in studies using objective measures should help validate the experiences of Veterans who have long noted a connection between their mental and physical health."
Cohen's findings are in line with those from a recent study led by Dr. Viola Vaccarino of Emory University. She worked with VA investigators to analyze data from the Vietnam Era Twin (VET) Registry. The VA-run registry includes some 7,000 middle-aged male twin pairs, all of whom served in the U.S. military during the Vietnam War.
The study looked at 562 Veterans—281 twin pairs—who had been followed an average of 13 years. It found that heart disease was more than twice as common among those with PTSD—about 23 versus 9 percent. When the researchers then conducted imaging tests with a radioactive tracer that shows blood flow to the heart, they found reduced flow among those with PTSD, even after adjusting for traditional cardiovascular risk factors and depression.
The group reported its findings in the Sept. 10, 2013, Journal of the American College of Cardiology.
Heart disease was one of several health problems that VA researchers found to be more common among those with PTSD in another study of Vietnam-era Veterans that appeared online in Quality of Life Research in December 2013.
Like Vaccarino's study, this one involved the Vietnam Era Twin Registry. But it relied only on mail surveys and telephone interviews and did not include any physical exams or imaging tests.
The study included 5,574 Veterans in all. Among those with PTSD, about 25 percent reported cardiovascular disease. For those without PTSD, the figure was 17 percent.
Ischemic heart disease—reduced blood flow to the heart—is the top cause of hospitalization among Veterans who use VA health care. Research has linked chronic PTSD to higher rates of ischemia, along with other heart conditions. (Photo by Warren Park)
Similar gaps in health status between those with and without PTSD were found across a range of physical and mental conditions, besides heart disease: diabetes, lung disease, depression, anxiety, alcohol use disorder. Those with PTSD also reported more disability.
The researchers, led by VA epidemiologists Dr. Jack Goldberg in Seattle and Dr. Kathy Magruder in Charleston, S.C., also found that combat exposure increased the risk of poor health and disability later in life, even in the absence of PTSD.
The findings "have potential implications for all combat-exposed Veterans," wrote the authors. "Physical and mental health treatment programs should consider both PTSD and combat experience."
The implication is that for warfighters, the experience of combat may register in the brain and nervous system as a trauma, even if the person never develops full-blown PTSD. And that trauma experience—like PTSD—may be enough to set in motion some physical disease processes.
In fact, according to Cohen, while some studies look at trauma exposure and others at PTSD, both approaches tend to produce similar findings, in terms of links to physical disease. One example is research tying trauma or PTSD to inflammation—a key factor in heart disease.
"There's enough evidence demonstrating that each is independently associated with inflammation," she says. "In addition, some studies show associations between early life trauma and inflammation many years later."
While most experts agree there's a strong link, maybe even a causal one, between PTSD and heart disease, theories abound as to how exactly that disease process works. Is the main culprit stress hormones that damage blood vessels over time? The bad health habits that tend to go along with PTSD, such as smoking and not exercising? Or poor sleep quality, which can thwart the immune system? In all likelihood, it's all of these and more, all interacting in complex ways.
Another question: Is there something unique about PTSD's effects on the heart, or is the same impact seen with related emotional problems, such as depression, anxiety, and hostility?
The links between those mental conditions and heart disease are well-documented. One recent study looked at the records of more than 236,000 Veterans and found a higher incidence of heart failure among those with depression or anxiety alone, or the combination of both. Past studies have found similar links to heart attack. Teasing out the impact of those conditions, versus that of PTSD alone, can be difficult. The consensus so far is that PTSD exerts an effect independent of any other conditions.
Dr. Mary Whooley , at the San Francisco VA Medical Center and UCSF, leads the Heart and Soul Study, which followed more than 1,000 heart patients for a decade. Her research has focused mainly on depression, not PTSD, but there are clear parallels.
She calls the relationship between depression and heart disease "complex and bidirectional," and suggests the same could be said of PTSD.
A couple of her papers have used a graphic that shows a circle with five boxes, with arrows going from one to the next. At the top is depression. The condition itself leads to harmful behaviors: inactivity, poor eating habits, social isolation, smoking, lack of adherence to medication regimens. These habits unleash a cascade of biological changes. They center on the autonomic nervous system, which controls heart rate and blood pressure, and which also triggers a release of stress hormones, involving the hypothalamus in the brain and the pituitary and adrenal glands. Other effects: Inflammation rises, blood vessels constrict, platelets clump together in the blood, raising the risk of clots.
This all contributes to cardiovascular disease. And that, in turn creates, physical health problems, difficulty with everyday tasks, money trouble, emotional distress.
The circle ends up back at depression. The cycle starts over again.
Says Whooley, "It's pretty obvious at this point that it goes both ways," referring to the link between depression and heart disease.
It wasn't always so obvious. For years, she says, the main focus of research was post-heart attack depression. It was clear that heart disease could cause depression. There was far less recognition of depression as a primary driver of heart disease in the first place. That view has changed.
What's getting the most attention now as a factor in heart disease, says Whooley, is the behavioral dimension of depression. A few of her studies have suggested that poor health habits "strongly contribute" to the development of heart disease.
"The emphasis is now on, well maybe this is a health behavior issue that can be modified, rather than a biological consequence we can't do anything about."
A similar dynamic, she notes, may apply in PTSD, with some key differences.
"Certainly there are different things that cause PTSD versus depression. And each may have different physiological responses that contribute to cardiovascular disease in different ways. For example, patients with depression often suffer from chronic anxiety, but patients with PTSD also tend to experience acute sensations of stress and panic that can impair blood flow to the heart. So stress-induced ischemia—low blood flow to the heart—is probably a more significant mechanism in PTSD than in depression."
At the same time, says Whooley, "There is likely to be significant overlap as far as how the two conditions are linked with heart disease. PTSD patients also have poor health behaviors, and these behavioral changes are linked to elevated inflammation and norepinephrine." Norepinephrine, also called noradrenaline, is a hormone released in response to stress.
Whooley's depression model, with its focus on poor health habits driving biological changes, may help explain, to a large extent, how PTSD damages the heart. But others place equal emphasis on how the emotional state of PTSD itself may directly vex the cardiovascular system.
One hallmark of PTSD is hyperarousal—feeling keyed up, on the lookout for danger. Another is mentally reliving the trauma, through flashbacks or nightmares. These symptoms, along with others, might set in motion the body's stress response, starting in the brain and orchestrated by the autonomic nervous system. Norepinephrine and other hormones are secreted, triggering changes throughout the tissues and organs of the body.
It's the "fight or flight" response, which is how the body responds to danger and threats. The heart beats faster, arteries constrict, blood pressure increases. The platelets in the blood become stickier, in preparation for clotting a potential wound. More glucose is pumped into the bloodstream, for quick energy. This can all save your life if you're being chased by a tiger. But when the process happens repeatedly over time, in response to chronic emotional stress, the lining of the arteries gets damaged. The heart muscle weakens. The effect is destructive, not protective.
Schnurr believes these direct biological links have a lot to do with PTSD's role in heart disease and other medical problems. But she doesn't discount the other mechanisms: poor health habits, for example, or related psychological conditions, such as depression or hostility.
The bottom line is, no one single mechanism seems to account for the relatively huge impact of PTSD on heart health and mortality. "We have links between stress and health," says Schnurr, "but we don't have the type of direct one-to-one links you might expect. And so it's hard to get from point A to point B."
To tie it all together, she likes to cite the "allostatic load" theory, first proposed in the late 1980s. "It seems like a good way to connect the dots," says Schnurr.
Allostatic load refers to the cumulative burden of stress. Every time the body goes through these many physiological changes to adapt to stress—some of them small and subtle—the experience adds to the overall wear and tear on the organism. It's like adding miles on your car and all its parts. Eventually, says Schnurr, "we pay a price.
"For the most part, the biological changes we see are not clinically remarkable. So it's hard to argue that any by themselves could lead to the types of physical health changes we see in PTSD. So conceptually, this theory makes sense."
There's another angle to consider: Do PTSD and heart disease share underlying risk factors that drive both conditions?
Some evidence points in this direction. A study of 2,600 Iraq and Afghanistan Veterans, for instance, suggests that pre-existing inflammation may contribute to an increased risk for PTSD. The results came out online Feb. 26 in JAMA Psychiatry.
The analysis is from the Marine Resiliency Study, supported by VA and the Marine Corps, Navy, and National Institutes of Health.
"Our study raises the possibility that those with higher levels of inflammation to begin with may be more vulnerable to developing PTSD symptoms, and those with less inflammation may be more resilient," says study coauthor Dr. Dewleen Baker, a psychiatrist with the Center of Excellence for Stress and Mental Health at the VA San Diego Healthcare System.
Baker and colleagues used pre-deployment measurements of C-reactive protein. The protein is made in the liver, and its levels in the bloodstream rise when there is inflammation in the body. In recent years, it has come to be used—along with triglycerides, cholesterol, and other measures—as a marker of heart risk.
Those Marines and sailors with higher C-reactive protein levels before they went overseas were more likely to have PTSD symptoms after returning from the war zone, and their symptoms tended to be more severe. Those with lower C-reactive protein levels at the outset seemed to show more resilience. They had fewer PTSD symptoms post-deployment, even with similar rates of trauma exposure.
One practical implication of the findings, says Baker, is that "any diet or lifestyle changes that reduce inflammation could, in theory, help lessen the severity of PTSD, or possibly help prevent the onset of symptoms in the first place."
She is quick to point out that the finding has to be replicated in further research, and she acknowledges that the link between mental health disorders and inflammation is complex.
Baker: "It's not unlikely that a vicious cycle does get set up"—like Whooley's model of depression and heart disease—"that predisposes not just to PTSD, but also to some of the medical comorbidities that are often found in chronic PTSD, such as atherosclerotic heart disease and metabolic syndrome."
Baker's group, along with others, has also studied a brain chemical called neuropeptide Y, which is measured in blood or spinal fluid. It's been called the "resiliency hormone." Research on Navy Seals and Green Berets has found they tend to naturally have high levels of the hormone in the blood in response to acute stress, and this could help explain their mental toughness and emotional resilience. Baker's team found lower cerebrospinal fluid levels of the peptide in people with PTSD, compared with those without the disorder. A 2013 study by another group showed that giving rats a dose through the nostrils right after a trauma could ward off PTSD-like symptoms. Interestingly, the hormone is also implicated as a factor in heart disease, although its exact role is not yet clear.
Another hormone, DHEA, which helps regulate stress and is known to play a role in preventing heart disease, is now being explored as a potential treatment for PTSD. A trial at the Bay Pines (Fla.) VA Medical Center is enrolling 120 Veterans. They will get a special, safe form of the hormone, which is sold as a natural supplement. Here, too, one underlying question is whether those with naturally lower levels of the hormone to begin with may be more susceptible to developing PTSD after a trauma.
Other researchers are exploring whether some of the same genes—further upstream in the biochemical pathway—help set the stage for both PTSD and heart disease.
Dr. Mark Miller , a psychologist and genetics researcher with VA's National Center for PTSD in Boston, has led genome-wide association studies comparing DNA from Veterans with and without PTSD.
Most of the discoveries by his team and others have focused attention on genes believed to play a wide role in human health, affecting many body systems.
"We've been turning up associations with genes that have been implicated in psychiatric conditions, but also in other types of health conditions, like cardiovascular disease or diabetes," says Miller.
He explains that's because the genes in questions help control systemic processes like inflammation and oxidative stress, which operate on cells and tissues throughout the body. So it's not a stretch to think that certain genes are ultimately affecting the risk for both PTSD and heart disease, as well as how each ailment plays out in the body.
A 2010 review study by a team at the Durham (N.C.) VA affirmed this theory: "It is possible that the genetic factors that predispose individuals to both conditions account for some or all of the association between PTSD and cardiovascular/metabolic disease," wrote the authors. The review was an exhaustive run-down of all the viable theories regarding the PTSD-heart connection.
Pinpointing the genes that play a role is only part of the challenge. Understanding how they interact with the environment—including a person's traumatic experiences—can get far more complicated. "Everyone's trying to get a handle on that," says Miller. "Ultimately, that's what it's all about."
Despite the seemingly infinite number of variables at play, Miller believes genomics will lead to practical insights to guide therapy. "The real promise of this research is identifying new biological mechanisms that we hadn't been thinking about in relation to PTSD, that we wouldn't have arrived at from a psychological theory of the condition. We can then target those pathways in the development of new treatments."
Whether or not genomics leads to new therapies for PTSD, the question still remains as to whether successful treatment of the condition translates into fewer incidents of heart attack, stroke, and heart failure. The evidence seems to suggest it should—and there are enough theories to explain why it should—but more research is needed.
Given the parallels between PTSD and depression, a 2011 study from the St. Louis VA was encouraging. It was led by Dr. Jeffrey Scherrer, who has done extensive database analyses on mental illness and heart disease. The study found that 12 weeks of antidepressant therapy was associated with lower rates of heart attack and death, although the researchers couldn't say for sure whether it was the easing up of depression that directly accounted for the lower heart risk.
No such broad finding exists yet for PTSD, but that could only be because no one has yet undertaken such a study—either in the context of a database analysis, or a clinical trial.
Says Cohen, "There haven't been any randomized controlled trials looking at the effects of PTSD treatment specifically on cardiovascular disease, to my knowledge, but the evidence we have suggests there is a dose-response relationship between PTSD symptoms and cardiac risk."
She cites several studies that seem to show a direct correlation between cardiac risk and PTSD severity. "This suggests—but doesn't prove—that if we could lower PTSD symptoms, perhaps we could slow down or even prevent cardiovascular disease."
According to Cohen, there have been a few studies tying PTSD treatment to "measures that we think might be mechanisms of cardiovascular risk." One, for example, showed reduced reactivity in the sympathetic nervous system, the part of the autonomic nervous system that mounts the fight or flight response. She calls this "preliminary evidence."
What's needed now, she says, are PTSD treatment trials that track heart outcomes more comprehensively.
"We need to start examining cardiovascular markers to see how they change with PTSD treatment in a trial setting. This would provide stronger evidence."
Also needed, she says, is "longitudinal epidemiologic research with repeated measures not only of PTSD symptoms but also cardiovascular disease and risk factors."
Schnurr adds a caveat: "PTSD may initiate the development of factors that lead to heart disease, but the heart disease itself many then take on a life of its own. I would suggest that treating PTSD would improve cardiac health only if the PTSD is causing 'maintaining' factors."
She explains, for example, that if poor health behaviors and stress are actively maintaining or worsening the heart disease, and treating PTSD can lessen those factors, that would lead to an improvement in heart health, and maybe even a reversal of some problems. "But once you have stenosis [narrowing of the arteries], I could treat your PTSD and make you symptom-free, but that won't treat the stenosis. You're going to have to do something else for that."
Either way, the good news, says Cohen, is the increasing emphasis—especially in VA—on blending mental and physical health care. Many VA primary care clinics now have mental health staff under the same roof, with screenings and counseling sessions or psychiatry visits built right into the primary care process, so Veterans don't have to come back another day or go to a different location. "It fits with our approach of taking care of the whole Veteran," she says.
Whooley concurs: "Overall, there's a shift toward integrating the mind and the body in all medicine. There's more recognition that mental health can affect cardiovascular health, and vice versa."
There are four types of PTSD symptoms:
Memories of the traumatic event can come back at any time. People with PTSD may feel the same fear and horror they did when the event took place.
Those with PTSD may try to avoid situations or people that trigger memories of the traumatic event. They may even avoid talking or thinking about the event.
The way people with PTSD think about themselves and others changes because of the trauma.
Those with the disorder may be jittery, or always alert and on the lookout for danger. They might suddenly become angry or irritable.
Adapted from www.ptsd.va.gov/public/PTSD-overview/basics/symptoms_of_ptsd.asp