Office of Research & Development |
 |
Office of Research & Development |
 |

VA Research Currents archive
January 7, 2015
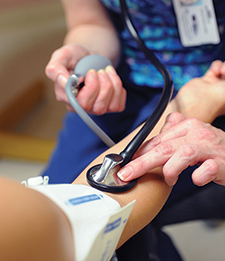
A variety of innovative treatment strategies is helping to improve blood pressure control rates among VA patients, says a new study. (Photo by April Eiler)
VA is getting better when it comes to managing Veterans' hypertension due to comprehensive, and sometimes creative, treatment methods. That's the gist of a new study aimed at quantifying the success of various behavioral interventions VA has in place to improve hypertension and blood pressure control.
Hypertension is the most common chronic condition in the VA population, affecting nearly 4 in 10 Veterans. It can lead to stroke and other deadly complications.
"High blood pressure can have all kinds of negative ramifications. It can exasperate existing comorbid conditions like diabetes," says Dr. Leah Zullig, a core investigator at the Center for Health Services Research in Primary Care at the Durham VA Medical Center in North Carolina. "It really is a silent killer, potentially decreasing people's lifespan, and it's easy to overlook because it can be symptomless at the early stages."
Zullig, also an assistant professor of medicine at Duke University, reviewed the results of 15 trials on hypertension control in VA. Specifically, she looked at what kind of behavioral interventions were in play at various VA facilities and what their success rates were.
The results appeared in the Journal of Clinical Hypertension in November 2014.
"When it comes to blood pressure and hypertension, there are things we can't control, like genetics. But with behavioral interventions, you're talking about diet, exercise, and other such factors that can make a difference in a person's health," says Zullig.
The indications overall are that VA is doing better at treating hypertension and controlling high blood pressure. Zullig cites a large VA study published in Circulation in 2012 that found that from 2000 to 2010, blood pressure control rates improved in VA from about 46 percent to 76 percent.
Part of that success, Zullig writes, is thanks to innovative behavioral approaches taken at many VA facilities. VA follows the Eighth Joint National Committee, or JNC-8, guideline for hypertension management, which uses the latest evidence to outline adult hypertension treatment. Nevertheless, there is flexibility within VA. Individual facilities may focus more on one treatment method over another.
"It really varies from institution to institution," says Zullig. "Durham might include telemedicine while another focuses more on group patient education. It's not always comparing apples to apples, and that's why this study is so important."
Zullig's research involved analyzing results from group hypertension treatment, self-monitoring by patients, medication-adherence plans, telehealth, early intervention, and even relaxation therapies.
"At VA, we deal with complex patients, but we do so taking that into consideration. The really successful treatments reflect that stance. They involve behavioral counseling, medication management, self-monitoring, and more. They address multiple issues."
While the solutions to high blood pressure and hypertension are as varied as the patients themselves, Zullig's research did identify common trends—such as increased frequency of contact. Also, group care was a big hit, with patients not only receiving access to clinical staff, but also having the opportunity to build peer support systems and friendships.
In one study involving 239 Veterans in North Carolina and Virginia with poorly controlled diabetes and hypertension, patients were assigned to seven- or eight-person groups led by a pharmacist, primary care internist, and nurse or other diabetes educator. Twelve months later, mean systolic blood pressure had improved by 13.7 mm Hg in group participants and by only 6.4 mm Hg in the usual-care patients.
Two other studies also evaluated group care. In one, four to eight participants underwent small-group training sessions for an hour. Led by a nurse, nutritionist, physical therapist, or pharmacist, the sessions proved more effective at controlling blood pressure than individual therapy, and at lower cost.
In yet another group study, nearly twice as many participants in group settings achieved their target hemoglobin goals, compared with their peers in individual therapy.
One of the more unusual studies reviewed by Zullig involved Veterans Service Organizations. The Posts Working for Veterans Health, or POWER study, used monthly sessions held at nine different VSOs throughout a given region so that at least one meeting a month would be conveniently located for a Veteran in the area. Peer leaders underwent training sessions and all posts received equipment such as scales, pedometers, and blood pressure monitors.
Other treatment methods involved nurse-administered home telehealth, remote monitoring, ramped-up education, personalized letters containing behavioral strategies, and more. According to Zullig, no matter how different the methods, they have one thing in common: an innovative mindset on the part of the providers, and a desire to improve Veterans' quality of life.
"We need to engage patients in their care and one way to do that is to bring attention to their status," says Zullig. "Often, just by making them aware, we can get them to engage in better behaviors in terms of what they eat and what they do."