Office of Research & Development |
 |
Office of Research & Development |
 |


More than 1.5 million Americans, including many Veterans, have inflammatory bowel disease. Symptoms can include severe diarrhea, abdominal pain, bleeding from ulcerations, and weight loss. (Photo for illustrative purposes only: ©iStock/Eva-Katalin)
February 1, 2018
By Mike Richman
VA Research Communications
What if doctors had a sort of “crystal ball” to predict flare-ups in patients with inflammatory bowel disease?
Such a tool could improve patient outcomes and save resources, say experts.
That’s the goal of Dr. Akbar Waljee, a gastroenterologist at the VA Ann Arbor Healthcare System in Michigan.
His research aims to improve the ability to predictlikelihood of someone with inflammatory bowel disease (IBD) experiencing intestinal inflammation, or a flare, that requires use of outpatient steroids or hospitalization. The predictions are based on patient record data, including a history of flares and changes in bloodwork, that identify patterns. This model essentially creates a tool that gives doctors a clearer idea of which patients to watch more closely, says Waljee, director of the inflammatory bowel disease program at the Ann Arbor VA.
His most recent study appeared in January 2018 in the journal Inflammatory Bowel Diseases.
Waljee says the model developed for the study has never been used in VA or non-VA settings.
“We are now able to predict the likelihood of a flare occurring and potentially intervene to prevent it by emphasizing the need to take medication consistently or change the medication,” he says. “This model could be used in clinic to identify patients at high and low risk for a flare, making it easier to tailor their care.”
With the ability to predict, Waljee and his team are hoping to avoid the need for outpatient steroid use and hospitalization. He says if someone is flaring that person will likely go on steroids. But he notes that steroids should be used only in emergencies and can cause bad side effects, including fractures, blood clots, and sepsis, an immune disorder that stems from the body’s inability to fight infection.
Instead, Waljee explains, the goal is to catch a potential flare early enough so it can be prevented through maintenance medications, such as adalimumab (sold as Humira), that suppress the immune system and thus stop the body from "essentially attacking itself." IBD is marked by unpredictable episodes of flares and periods of remission, making medical decisions tricky. Tools that can accurately predict disease course can substantially aid therapeutic decision-making, according to Waljee and his colleagues.
"I first encountered inflammatory bowel disease as a medical student and was struck by the profound impact it can have on the lives of patients and families."
Because drugs can take two to three months to take full effect, it is important to catch a pending flare at least three months in advance, Waljee notes.
Stool tests produce the most commonly used biomarkers to predict intestinal flares. Some of these tests are not widely available, are expensive, and have varying accuracy. The popular fecal calprotectin test, for example, can predict flares up to 12 weeks out. But it’s normally used to detect if a flare is happening “right now,” says Waljee, who is also an associate professor at the University of Michigan.

VA researcher works to improve antibiotic prescribing for Veterans

Veteran interest in Gulf War Illness reflected in new research study
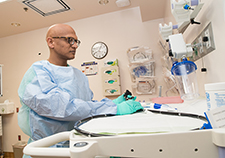
Study: Delaying colonoscopy following abnormal stool test increases risk of colorectal cancer
“Without the ability to accurately predict future flares, many patients suffer disabling or even fatal disease exacerbations when earlier stepping up of treatment could have kept them in remission,” he and his colleagues write. “[Some] patients undergo long periods of ineffective or unnecessary maintenance therapy when they might have benefited from an opportunity to [scale back] therapy.”
More than 1.5 million Americans, including many Veterans, have inflammatory bowel disease.
The term refers to Crohn's disease, a chronic inflammatory condition of the gastrointestinal tract, and ulcerative colitis, an inflammation limited to the colon. Both conditions often involve severe diarrhea, abdominal pain, bleeding from ulcerations, and weight loss. They can sometimes lead to life-threatening complications.
In 2014, costs from IBD in the U.S. ranged from $14.6 to $31.6 billion, most of which was due to outpatient pharmaceutical fees and hospitalizations.
This economic pattern is also seen with other inflammatory diseases, such as rheumatoid arthritis, lupus, and multiple sclerosis. Those diseases are often diagnosed early in life and require lifelong treatment, with patients suffering complications that can lead to high lifetime costs and premature death.
Inflammatory bowel disease is sometimes confused with another potentially debilitating intestinal disorder: irritable bowel syndrome. IBD involves an immune imbalance in any part of the gastrointestinal (GI) tract, resulting in lifelong, recurring inflammation. It can lead to abscesses and cancers. Some patients require surgery.
Irritable bowel syndrome causes GI tract pain, diarrhea, constipation, abdominal bloating, and bowel urgency. But it’s not an inflammatory condition and usually doesn’t lead to bowel damage or surgery.
Waljee doesn’t have inflammatory bowel disease, nor do any of his family members. But he knows how critical it is to treat patients with IBD in a timely and effective way.
“I first encountered inflammatory bowel disease as a medical student and was struck by the profound impact it can have on the lives of patients and families,” he says. “IBD can occur in anyone, even at a very young age, and can have devastating disease- and medication-related complications. This life-long disease requires medications that are, at best, 70 to 80 percent effective, can have burdensome side effects, and are often quite expensive. Anything we can do to improve IBD disease outcomes and quality of life for Veterans is very important to me.”
In addition to caring for patients with IBD, Waljee is interested in using data to help doctors provide the right care to the right patient at the right time. He hopes to achieve this type of personalized health care through his research. His latest study connects his interests in inflammatory bowel disease and personalized care.
Using VA data from 2002 to 2009, Waljee and his team collected details about Veterans at a particular time point, namely a clinic visit or a lab visit. The team identified more than 20,000 patients who had been treated for IBD in the VA system. More than 50 percent of the patients had ulcerative colitis, and 35 percent had Crohn’s disease.
The patients, almost all of whom were men, averaged 59 years in age.
The researchers based their model on clinical and lab findings to predict IBD hospitalizations and outpatient steroid use. They used many variables to construct the model. The five strongest predictors of a flare were the patient’s age, the mean albumin, the mean platelet count, the highest platelet count, and any past use of steroids.
Albumin is a protein that keeps fluid from leaking out of blood vessels, nourishes tissues, and transports hormones, vitamins, drugs, and other substances through the body. Platelets are blood cells that help form clots to stop bleeding.
Waljee and his team predicted, with about 80 percent accuracy, which patients in the next six months would need steroids or IBD hospitalization. In comparison, the fecal calprotectin test, which requires patients to produce a stool sample using an equipment kit and bring it to a clinic for testing, is 71 percent accurate, according to the researchers.
“Once validated for general use, such a model has far-reaching clinical and research implications,” the researchers write. “The model offers a simple, inexpensive tool that can be used at the point of care by clinicians to tailor IBD treatment, as well as by health systems or clinical coordinators for systems approaches to quality improvement.”
Waljee wasn’t surprised by the results of the study.
“The way I like to think about this is that your body responds to any injury, medication, or disease by making a variety of changes internally,” he says. “This can result in changes to your blood counts or chemistries that may provide a more accurate reflection of health. The fecal calprotectin, like any test, is not 100 percent accurate. We hypothesized that measuring some patterns in readily available lab tests may be more predictive.”
Waljee says he’s excited about using the model to help patients avoid flares. But before putting the method into practice, he must prove it works in a clinical setting.
He’s planning to launch a follow-up study to evaluate the model in clinic and compare it to the current standard of patient care, which would most likely be a stool test.
“My hope is to implement the model at VA after additional evaluation, intervention development, and partnerships are formed,” Waljee says.
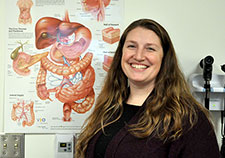
Nicole Bundas, an Army Veteran and Human Resources staffer at the Ann Arbor VA, was diagnosed with Crohn’s disease a decade ago, when she was training at Fort Dix for a year-long deployment to Iraq. (Photo by Brian Hayes)
For Army Veteran Nicole Bundas, life is a constant game of anticipation.
As someone with Crohn’s disease who has frequent bouts of diarrhea, she always has to plan where she is in relation to a restroom. The number of her trips to the restroom depends on whether she’s experiencing intestinal inflammation, or a flare. If that’s the case, she says, it could be more than five per day.
Crohn’s disease and ulcerative colitis are the two forms of inflammatory bowel disease (IBD).
“It’s really been a struggle for me, especially at work, having to realize that this disease changes your life,” says Bundas, who is also a former member of the Michigan National Guard. “Most people can just get up and go, kind of, `I can just go on a trip.’ Nobody wants to go to the restroom multiple times and possibly have an embarrassing accident or something like that in your place of business. So you think about that more.”
Bundas, 36, praises her colleagues at the VA Ann Arbor Healthcare System in Michigan, where she works in human resources, as well as her family, for being supportive of her.
She notes that her three kids, all of whom are under age 15, must always be on their toes.
“When mom says we’ve got to go, it’s because I need to get to a bathroom,” she says. “Or if I drop everything and run, it’s not that they’ve done something wrong. It’s just that I have an emergency, and I’ve got to go.”
Bundas was diagnosed with Crohn’s disease in 2008. At the time, she was experiencing extreme abdominal pain and cramping while training at Fort Dix in New Jersey for a year-long deployment in Iraq. She consumed a high-carb diet that included many ready-to-eat meals and was under a lot of stress as a single mom preparing to leave two kids for a tour in Iraq, where she served at a joint forces press center in Baghdad.
Bundas falls into one of the two age groups that are most impacted by IBD: patients diagnosed between 20 and 40 and those between 60 and 80. Many post-9-11 Veterans like her are in the 20 to 40 group. But the high-carb diet they consumed to support their rugged physical activity in the military didn’t necessarily trigger their disease, says Dr. Akbar Waljee, a gastroenterologist at the Ann Arbor VA who is treating Bundas.
No one has been able to pinpoint what causes IBD, Waljee notes. He says genetics, smoking, diet, infections, and drugs are all factors that can make one more susceptible. “But it’s not one thing,” he emphasizes.
Bundas says two other members of her family have Crohn’s disease and three others have ulcerative colitis. Still, doctors have been unable to determine if a specific gene or marker caused her Crohn’s disease, she says.
In the case of diet, Waljee says there’s no one-size-fits-all solution for someone with IBD. Foods typically high in carbs and greens like lettuce that are hard to digest tend to worsen symptoms, although some people may be fine with a carb-rich diet, he says. Bundas is on a low-carb, low-sugar diet because she says it helps reduce the inflammation.
Her medication consists of two immunosuppressive drugs that control intestinal inflammation. One of them also prevents the formation of antibodies.
Waljee hopes the model tested in his latest study (see main story) will be able to predict an oncoming flare and enable patients to get on maintenance medications, to avoid major inflammation.
Bundas appreciates that Waljee is seeking new ways to prevent IBD flares.
“I know not everyone can be seen at the Ann Arbor VA because not everybody’s a Veteran,” she says. “But for those who are, or if you’re going to see a doctor outside, look for someone who is continuing to move forward and is on the cutting edge of things and not just sitting back and doing things how they were always done. We need to stay on the cutting edge in medicine because that’s how we’re going to continue to make progress.”
—Mike Richman
VA Research Currents archives || Sign up for VA Research updates