Office of Research & Development |
 |

VA Research Currents archive
March 9, 2017
By Tristan Horrom
VA Research Communications
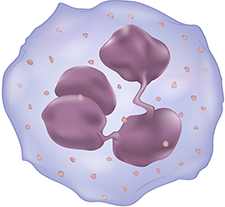
Neutrophils—the most prevalent white blood cells in the body—undergo structural and functional changes when infected by Helicobacter pylori bacteria, found a VA-University of Iowa research team. (Photo: ©iStock/blueringmedia)
Researchers with the Iowa City VA Health Care System and University of Iowa have produced striking new evidence of neutrophil plasticity, or the ability of these white blood cells to change their properties.
The scientists exposed neutrophils—the most prevalent white blood cells—to Helicobacter pylori bacteria, a common source of infection in the U.S. and worldwide, and the cause of stomach ulcers and other gastric problems. The lab experiments are among the first to show how mature white blood cells can change while still alive, in response to bacteria.
"Changes in neutrophil phenotype [observable traits] and function have been observed before, but only in vivo—such as in the circulation of sepsis patients, or in the joints of persons with arthritis," said study senior investigator Dr. Lee-Ann H. Allen. "However, previous attempts to reproduce these phenotypes using neutrophils isolated from human blood have not been successful. Thus, our study is the first to show that H. pylori infection, on its own, can alter the phenotype of human neutrophils."
"Our study is the first to show that H. pylori infection, on its own, can alter the phenotype of human neutrophils."
Allen and her colleagues say the new findings may lead to a better understanding of how bacterial diseases arise in the body and how white blood cells respond. The scientists believe this may pave the way for new treatments, especially in the area of gastric health.
The results appeared March 1, 2017, in the Journal of Immunology.
Neutrophils are the most common white blood cells in the human body. The concepts of neutrophil plasticity and different neutrophil phenotypes—cells with different structural characteristics and functions— have emerged only in the past few years. Previously, scientists thought these cells all had similar properties. But recent studies found different subsets of neutrophils in the body. However, no experiments until now were able to replicate the development of different neutrophil types in the lab.
In the new study, the Iowa researchers exposed neutrophils from human blood to H. pylori bacteria. H. pylori is a common bug that infects the human stomach. It can cause gastritis, peptic ulcers, and gastric cancer. H. pylori infection usually causes chronic inflammation, with a neutrophil-rich response from the immune system.
The neutrophil cells exposed to H. pylori underwent structural changes. The nucleus of a normal neutrophil cell usually has three or four interconnected lobes. But when infected with H. pylori, the neutrophil nuclei showed six or more lobes per cell.
Such "hypersegmentation" is rare in neutrophils. According to the researchers, it shows the bacteria are actively changing the neutrophils through a direct interaction.
Hypersegmentation was not seen when the researchers exposed eosinophils, a different type of white blood cell, to H. pylori. Also, the change only happened when neutrophils were directly infected with H. pylori, rather than when the bacteria were merely present. Neutrophils exposed to E. coli did not develop hypersegmentation, suggesting the change could be specific to H. pylori.
The phenotype change, rather than support a stronger immune response, appears to help the bacteria survive. Altered neutrophils do not kill H. pylori cells.
The bacteria also change the neutrophils in other ways, the study found. Normal neutrophils die as part of a natural process. But infected cells lived longer. The infected neutrophils also released molecules that are toxic to surrounding cells. When neutrophils are functioning normally, they produce chemicals called reactive oxygen species (ROS) around bacteria to kill the infection. H. pylori manipulates neutrophils so that they release ROS into the space outside the cells instead. This damages the stomach cells and helps the infection survive and spread.
The picture is not all bad, though. The changes brought on by H. pylori may also curtail gastric cancer. While H. pylori is classified as a carcinogen, it mainly causes gastritis and only rarely triggers ulcers or cancer. The hypersegmented neutrophils share some characteristics with tumor-associated neutrophils (TANs) in mice, found the study. Evidence suggests that abundant TANs are beneficial in human gastric cancer patients. So if the presence of this type of neutrophil really does limit tumor growth, it would help explain how H. pylori is able to chronically infect humans without resulting in gastric cancer in every patient. It also suggests that manipulating neutrophil phenotypes could possibly help treat gastric cancer.
The new study is the first lab demonstration of bacteria manipulating mature neutrophils. The authors say the work highlights the intriguing properties of these immune cells. They write, "Our findings are noteworthy as there is convincing evidence that [neutrophils] have multiple and potentially paradoxical roles in the development and progression of gastric disease."
The VA and University of Iowa researchers now plan to test other bacteria species to see if they have similar effects. The idea of neutrophil plasticity is still in its infancy, and the team says more research will lead to a better understanding how pathogens such as H. pylori interact with neutrophils or other white blood cells, and how the process can possibly be harnessed to fight disease.
The study was funded by the National Institutes of Health.