Office of Research & Development |
 |
Office of Research & Development |
 |


Pulmonary oncologist Dr. Catherine R. Sears meets with VALOR clinical trial participant Mr. Bobby Richardson. (Photo by Mark Turney, Richard L. Roudebush VA Medical Center.)
March 30, 2021
By Erica Sprey
VA Research Communications
"Early screening is essential to increasing the number of long-term lung cancer survivors."
Each year, over 8,000 Veterans are diagnosed with lung cancer in the U.S.
It is the second most common type of cancer in the nation—affecting over 235,000 individuals each year, according to the American Cancer Society. It is also the leading cause of cancer deaths in both men and women.
The Veterans Affairs Lung Cancer Surgery Or Stereotactic Radiotherapy (VALOR) clinical trial, sponsored by VA, is evaluating the effectiveness of two different types of treatment for lung cancer— surgery vs. targeted radiation therapy. As patients are screened and found to have lung cancer, qualified individuals are offered the chance to enroll in the study. Investigators hope to find out which treatment results in a better five-year survival rate for stage 1 non-small cell lung cancer (NSCLC).
Study locations currently include the following VA medical centers: Long Beach, California, Bay Pines, Florida, Atlanta, Hines, Illinois, Indianapolis, Minneapolis, Durham, North Carolina, Pittsburgh, Houston, and Richmond, Virginia. Investigators hope to enroll 670 participants.
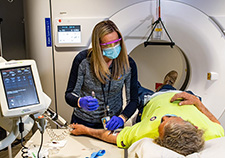
Medical imaging supervisor Christine Thalheimer assists Vietnam Veteran Mr. Bobby Richardson during his CT scan. (Photo by Mark Turney, Richard L. Roudebush VA Medical Center.)
Historically, surgery to remove cancerous tissue has been the standard for treatment of stage 1 non-small cell lung cancer. However, surgery can be physically taxing for some patients, especially people who are elderly. Given that the average age of diagnosis for lung cancer is about 70, advanced age can be a significant factor in patient survival.
A newer treatment—Stereotactic Body Radiation Therapy (SBRT)—delivers high-dose X-rays that are targeted to cancerous cells in the body. SBRT is an FDA approved treatment for lung cancer. In frail or elderly patients, the therapy is much easier to tolerate compared to surgery. SBRT requires three to five visits each week, for one to two weeks.

VA researchers using AI to decide best treatment for rectal cancer

Dr. Christopher Slatore
Lung cancer

VA Study Documents Health Risks for Burn Pit Exposures

Dr. Siddiqui
Prostate cancer screening
While both surgery and SBRT can cure stage 1 non-small cell lung cancer, no large studies have compared the effectiveness of these two therapies in patients who are healthy enough to get surgery. VA researchers aim to collect data that will help physicians choose the most effective treatment for each individual.
Dr. Drew Moghanaki, a radiation oncologist and co-chair for the VALOR study, believes that providing more options for patients with lung cancer is critical. "If we had data that showed that surgery or radiation therapy was better for a given patient, then we would be able to use safety and other criteria to decide which treatment to give," he says. "We would have more options to better match each patient to the optimal treatment for them."
Lung cancer deaths are declining, in part, because fewer people smoke and there have been significant advances in treatment and early detection programs.
There are a number of initiatives within VA that aim to detect lung cancer early enough to effectively treat the disease. Thanks to the combination of earlier detection paired with cutting-edge research on new treatments, VA hopes to make a difference for Veterans affected by cancer.
Providing lung cancer patients with multiple treatment options is an important component of VA's National Oncology Program. However, equally important is the widespread adoption of early screening programs for lung cancer, both within and outside VA.
In addition to his other roles, Moghanaki is the director of the VA Partnership to increase Access to Lung Screening or VA-PALS. It is a nationwide program that has increased the number of Veterans who are screened for lung cancer. Moghanaki says that VA has become a leader in lung cancer screening.
When lung cancer is caught and treated in the earliest stages, patients have a better chance of survival and quality of life. According to the American Lung Association, detecting lung cancer early before it spreads can increase a person's likelihood of surviving for five years by 51%.
The U.S. Preventive Services Task Force has expanded its recommendation for annual lung cancer screening to current or former smokers—who quit within the last 15 years—who are 50-80 years old, with a 20 pack-year smoking history. One pack year is equal to smoking one pack of cigarettes a day, for one year.
"Early screening is essential to increasing the number of long-term lung cancer survivors—similar to the success of early screening programs for prostate or breast cancer. Now with greater adoption of lung cancer screening programs and innovative treatments like immunotherapies, all of that is changing," notes Moghanaki.
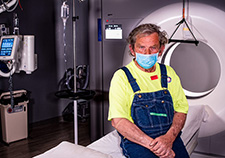
Lung cancer survivor Mr. Bobby Richardson receives follow-up care at the Richard L. Roudebush VA Medical Center in Indianapolis. (Photo by Mark Turney, Richard L. Roudebush VA Medical Center.)
Vietnam Veteran Bobby Richardson can attest to the effectiveness of early screening for lung cancer. Last year, he found out that he had stage 1 lung cancer and was treated through a VA clinical trial called Veterans Affairs Lung Cancer Surgery Or Stereotactic Radiotherapy (VALOR).
The 69-year-old resident of Bloomfield, Indiana, says his VA physician recommended screening for lung cancer based on his family history. Several aunts had died from cancer, and Richardson had just lost his brother to advanced lung cancer. Then, following his own diagnosis, his sister was diagnosed with a different form of cancer.
"My brother didn't have any symptoms up until the last year before he found out that he had lung cancer. He kept complaining that something was wrong. His doctor said, 'You are just getting emphysema,'" says Richardson. It wasn't until Richardson's brother switched his care to VA that he was diagnosed with stage 4 lung cancer.
Richardson, who drives a lumber truck for a living, says he was happy to participate in VA-PALS. "I was glad to do it because cancer runs in my family. That way I didn't have to worry about it." He says his doctors caught his cancer early when it was still treatable.
After screening positive for lung cancer, Richardson was enrolled in the VALOR study at the Richard L. Roudebush VA Medical Center in Indianapolis. His doctor, Dr. Catherine Sears, is the local site investigator for the VALOR clinical trial and director of the VA-PALS screening program at Indianapolis.
One year after treatment, Richardson is cancer-free. He will undergo follow-up care in VA for five years. He says he's one of the lucky ones. "My experience was pretty positive because my doctors cured me. The thing of it was, I never felt sick, never felt bad. I didn't even know that I had cancer, until they told me. I would definitely recommend that other Veterans get screened."
VA Research Currents archives || Sign up for VA Research updates