Office of Research & Development |
 |

VA Research Currents archive
April 5, 2017
By Mike Richman
VA Research Communications
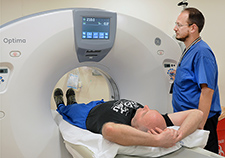
CT scanners like this one at the Durham VA Medical Center, staffed by technologist Robert Jacobsen, are at the core of lung cancer screening programs. VA is reviewing options for implementing screening at its facilities nationwide. (Photo by Linnie Skidmore)
It's no secret that thousands of Veterans are current or former smokers, a major reason why lung cancer is one of the most commonly diagnosed cancers in the VA system. So what about a screening program, using lung imaging, to detect those affected by or at risk for the disease?
Sounds like a vital undertaking. But it's not that simple.
That's the finding in a VA study that says developing and implementing a comprehensive lung-cancer screening (LCS) program for the nearly 900,000 Veterans who are eligible is "complex and challenging, requiring new tools and patient care processes for staff, as well as dedicated patient coordination."
The study appears in the March 2017 issue of JAMA Internal Medicine.
"For example, creating electronic tools to capture the necessary clinical data in real time that met the needs of the LCS coordinators proved to be difficult, even with the VHA's highly regarded electronic medical record," the researchers write. "Although computerized clinical reminders about current or recent smoking are widely used in the VHA, more detailed information about pack-years smoked and years since quitting was required. This information is not fully captured in the electronic medical record."
Lead author Dr. Linda Kinsinger says there are staff- and patient-related difficulties with carrying out such a voluntary program. Just getting patients to keep appointments for screenings and follow-ups is a major challenge in itself, and one that could lead to logistical hardships, she says. No data were kept on the number of appointment cancellations, but she says the lung cancer screening coordinators told of many such instances.
"We wanted to find out how easy or hard it would be [to implement a screening program]. It turned out to be a lot more complex than we had hoped."
"It's not just asking, 'Do you want your flu shot,' " Kinsinger says. "It's a much more difficult conversation. As with anything, you can make appointments, but people sometimes don't show up when they're supposed to. So then you have to stay on top of that to get them rescheduled. We had lots of recalls in the study, so that meant more appointments and more scheduling and more decision-making by the patients on whether they really want to follow up on this. It turned out to be lots of steps for staff and patients."
A recall pertained to patients who had at least one nodule, an abnormal swelling on the lung, found on the screening exam. They were asked to return in three, six, or 12 months for a repeat study to see if the nodule was growing or changing.
Kinsinger, who retired last year from VA after serving as VA's chief of preventive medicine at the National Center for Health Promotion and Disease Prevention in Durham, North Carolina, says she wasn't surprised by the final conclusions.
"We wanted to find out how easy or hard it would be," she says. "It turned out to be a lot more complex than we had hoped. It just involved so many different steps, people, handoffs, and technical requirements. So it became clear fairly early on in the course of the demonstration projects that this is complicated."
The origins of the study are linked to the National Lung Screening Trial. That landmark study aimed to compare the effectiveness of low-dose helical computed tomography, or a CT scan, versus a standard chest X-ray. The former uses X-rays to obtain a multiple-image scan of the chest, while a standard X-ray produces one image and is less powerful than a CT scan. According to trial results released in 2011, deaths in the CT scan group were 20.3 percent lower than in the X-ray group.
The screening trial led to a 2013 recommendation by the U.S. Preventive Services Task Force for annual lung cancer screening using a CT scan for current and former heavy smokers 55 to 80 years old. Based on that recommendation, the National Center for Health Promotion and Disease Prevention called for Kinsinger's Lung Cancer Screening Demonstration Project.
Patients in the project were identified for consideration at eight VA hospitals. Those age 55 to 80 without a diagnosis of esophageal, liver, pancreatic, or lung cancer, and without a life expectancy of less than six months, were singled out through VHA electronic records. Nurses then identified current and former smokers who had amassed at least 30 pack years: number of packs per day times the number of years smoked. A former smoker was someone who had quit less than 15 years ago.
The 2,106 participants underwent lung cancer screening from July 1, 2013, to June 30, 2015. Most of them had one round of screening. Ninety-six percent of the patients were men.
Across the eight sites, 1,257 (59.7 percent) of the patients tested positively, including
1,184 (56.2 percent) who had at least one nodule that needed to be tracked. Seventy-three patients (3.5 percent) had findings suspicious for possible lung cancer and underwent more evaluation; 42 (2.0 percent) required further evaluation, but the findings were not cancer; and 31 (1.5 percent) had lung cancer. The scans of 857 patients (40.7 percent) noted incidental findings such as emphysema, other pulmonary abnormalities, and coronary artery calcification.
Kinsinger says 20 of the 31 lung cancers were in stage one. "If we had found that the majority of them were in stage three or four, I think it's a closed case, there's no reason to do it," she says. "But, in fact, two-thirds were in stage one, so that sort of weighs more toward some possible benefit here." Early detection has been shown to improve outcomes for lung cancer patients.
Initially, more than 93,000 primary care patients were assessed on screening criteria, and 4,246 met the criteria and were offered screening. But only 2,452 (58 percent) agreed to do it. (Of those, 346 were excluded because they failed to undergo a scan within the project's time frame.) The patients' reasons for not agreeing to participate weren't collected but may have included concerns such as exposure to radiation, psychological distress, and the effort required to undergo screening.
The researchers estimate that if the eligibility figure found in the project is representative of the VA population, then nearly 900,000 Veterans would meet the screening criteria for age, smoking history, and medical history.
"The number of Veterans who may be candidates for annual LCS is substantial," the researchers write. "Accurately identifying these patients and discussing with them the benefits and harms of LCS will take significant effort for primary care teams. Based on [the demonstration project], only about 58 percent of candidates will agree to be screened." That decline may be frustrating for the screening coordinators who invest the time to identify the nearly 900,000 candidates, Kinsinger says.
"I don't know how to get around it," she says. "I wonder what the uptake rate for colorectal cancer screening is, as a comparison. It's the nature of screening tests."
Kinsinger and her team laid out a series of other potential obstacles with a national program:
"Implementation of a comprehensive lung cancer screening program requires significant clinical effort for as-yet uncertain patient benefit," the researchers write.
The researchers didn't look at possible psychological harms from lung cancer screening. But a 2015 study led by Dr. Steven Zeliadt of the VA Puget Sound Health Care System in Seattle found that screening can make people less motivated to quit smoking.
Kinsinger explains that some smokers in Zeliadt's study became complacent.
"[Zeliadt] interviewed some of the patients who had been in our demonstration project about their interest in quitting smoking," she says. "Interestingly, he found that some of the ones who were still smoking, if they had a negative scan, they said, 'I'm good, I can keep smoking.' And if they had a scan that showed a nodule or an incidental finding, they said, 'Well, that's good that they found it. They can look into it and follow it, and I can keep smoking.'
"So there's a concern there that the message about quitting smoking, which is certainly the most important message in terms of lung cancer prevention, may get lost in a, 'Well, I'm in a screening program, so I'm okay,' kind of a situation," she says.
Kinsinger says a national program would call for patients to undergo annual screening for many years. If a smoker enters the program after quitting 10 years prior, for example, then he or she will be screened for five years. Current smokers will undergo annual screening for as long as they continue to smoke, plus up to 15 years. The age cap for participants will be 80.
So faced with these challenges, will VA be implementing a national lung cancer screening program? Dr. Jane Kim, a co-author of Kinsinger's study and VA's current chief of preventive medicine at the National Center for Health Promotion and Disease Prevention, indicated that the program is under discussion.
"VA's Central Office is currently considering lung cancer screening guidance and recommendations for facilities, and is reviewing resources and tools that may be helpful in implementation of lung cancer screening," she says.
Kim gave no timeline for a possible start date.