Office of Research & Development |
 |

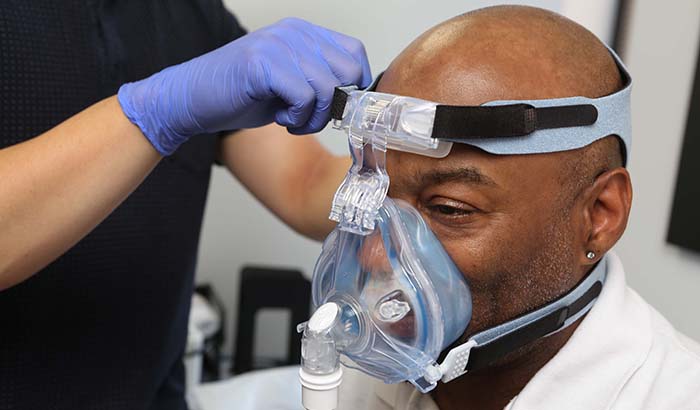
Ralph Liggins tries on a CPAP mask at the Jesse Brown VA Medical Center in Chicago. (Photo by Jerry Daliege)
June 28, 2017
By Mitch Mirkin
VA Research Communications
At 5 feet 7 inches tall and 165 pounds, Ralph Liggins is a fit 54-year-old who looks more like a middleweight boxer than your typical patient with obstructive sleep apnea. The condition usually affects heavier people.
But the former Air Force mechanic has been coping with the ailment for some 15 years and has it "really bad," he says.
"My kids don't want to sleep near me. They tell me I snore bad," says Liggins, now a special-education teacher.
He is used to getting by on five or six hours of sleep a night, "and out of that about an hour and a half I toss and turn."
A recent participant in a study at the Jesse Brown VA Medical Center in Chicago, Liggins learned that his breathing stops some 27 times per hour when he sleeps.
"About every three minutes, I stop breathing. I guess it doesn't stop for too long, because I'm still here."
The frequent mini-breaks in breathing wreak havoc on the body's autonomic nervous system and cause the heart to work harder. What's more, each time breathing stops, the brain sends a subtle wake-up signal to the sleeper, to make sure breathing resumes. As Liggins can attest, the result is sleep that is broken and not restful.
"About every three minutes, I stop breathing."
When not treated effectively, sleep apnea can cause a downward spiral in overall health. High blood pressure and other forms of heart disease can worsen. The risk of diabetes and depression go up. And as patients struggle to function on little sleep, they risk getting into car crashes or work accidents.
Liggins and other African-Americans, especially men, are at higher-than-average risk for the condition. But they are less likely than non-minorities to use the gold-standard treatment for sleep apnea, a continuous positive airway pressure (CPAP) machine. CPAP users wear a mask while they sleep that gently forces air into the throat. That keeps the airway from collapsing, which is what causes breathing to stop. The device also helps snuff out snoring.
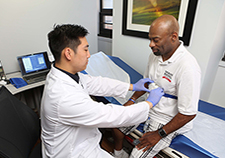
Research technician Michael Tam fits a finger probe on Ralph Liggins, part of a system that will monitor his sleep at his home. (Photo by Jerry Daliege)
Dr. Bharati Prasad, a pulmonary, critical care, and sleep medicine physician at the Jesse Brown VA, is well-versed in the literature showing that African-Americans are not using CPAP therapy to full advantage. At the same time, she finds it striking that with better adherence, blacks can actually benefit even more dramatically than other groups.
"When I started with this work, we did a retrospective observational study in Veterans, and we found that when adherence was comparable between the groups, blood pressure actually responded better in African-Americans than in whites."
That drove her to design her latest study, the one Liggins enrolled in. It's funded by a VA Clinical Sciences Research and Development Career Development award. The goal is to probe deeper into the potential benefits of CPAP for African-Americans, especially with regard to blood pressure. It will involve 220 Veterans—160 who self-identify as African-Americans, and the rest from other races.
"There's a very big gap in using the equipment," says Prasad, referring to the racial disparity between whites and blacks. "The benefits related to CPAP treatment, including with regard to blood pressure, are very directly and tightly linked to the length of treatment, and the appropriate use of the treatment."
By "length of treatment," Prasad means nightly use of the machine, versus more sporadic use.
Participants in the study get extra attention to help ensure they are using their CPAP machine appropriately, but they also go through specialized testing.

Their blood pressure is tracked more closely than would occur in routine clinical care. Rather than looking at a one-time snapshot of blood pressure, Prasad wants to see what happens to their pressure throughout the day and night, including during sleep. The participants wear a monitor that takes readings every half hour or so, during a 24-hour period.
"This is very important in sleep apnea," she says, "because when you sleep, your blood pressure isn't going lower the way it should normally."
The study volunteers also get their aortic blood pressure measured: A probe is placed on the neck, on the carotid artery, and a cuff around the thigh measures pressure in the femoral artery. "This looks at the blood pressure nearer to the level of the heart," explains Prasad, "and calculates the stiffness of the central arteries." Stiffer arteries are not good for heart health.
There are also urine tests to measure hormones involved in the body's stress response, as well as DNA tests to validate ancestry. That will help Prasad's group tease out the role of race per se in sleep apnea and CPAP response, versus related socioeconomic factors (see sidebar).
Last but not least, study volunteers fill out questionnaires about daytime sleepiness, and perform an alertness test using a clever handheld device.
"We're doing our best with all the noninvasive measures at our disposal," says Prasad.
As the study progresses, Prasad hopes to collect some of the strongest data yet on the link between CPAP adherence and blood pressure in African-Americans.
She says the evidence will help lay the foundation for more targeted treatment of sleep apnea in this high-risk population.
Liggins, for one, is still struggling to make CPAP work for him. He's been using it about four months, but hasn't quite adjusted. He acknowledges it helps somewhat with his sleep apnea symptoms and has improved his sleep a bit overall. But even with a well-fitted mask, he says, he finds the device uncomfortable. He usually ends up wearing it only three or four nights a week.
"You feel like you have something on your face," he says. "You know it's there."
He's says he's looking into trying a CPAP machine with a different type of mask.
Sometimes the cause of his lack of adherence is rather simple, and somewhat ironic: He's just too plain tired.
"Sometimes when I get home I'm so tired, I just fall asleep and forget to put it on."
Sources: American Sleep Apnea Association, National Sleep Foundation
Asked to explain why it is that African-Americans with sleep apnea are less likely to use CPAP therapy than other groups, Dr. Bharati Prasad says "there are likely a number of reasons." She says cultural factors like mistrust may play a role. "It has to do with understanding the disease, accepting the treatment, and finally using the treatment. Even when African-Americans have the equipment in their home, they still tend to not use it as much."
Her remarks reflect evidence from various studies, such as a 2011 study by VA researchers and university partners in which blacks had lower adherence rates than whites to CPAP therapy—despite efforts to standardize treatment, in the context of a well-controlled clinical trial.
The reasons, noted the researchers, are complex. While race by itself did independently predict lower adherence rates, socioeconomic factors likely play a role as well. The study authors wrote:
"Individuals with low socioeconomic status (SES) and those of minority race/ethnicity have higher levels of obesity, physical inactivity, alcohol consumption, smoking, and poor medication compliance; these health behaviors may correlate with CPAP adherence...Barriers to adherence in low SES groups may include low health literacy, competing needs with limited resources, and limited access to care."
More recently, in 2016, a Brigham and Women's Hospital study concluded that "the reasons for these disparities...are not well understood and should be a research priority."
VA Research Currents archives || Sign up for VA Research updates