Office of Research & Development |
 |

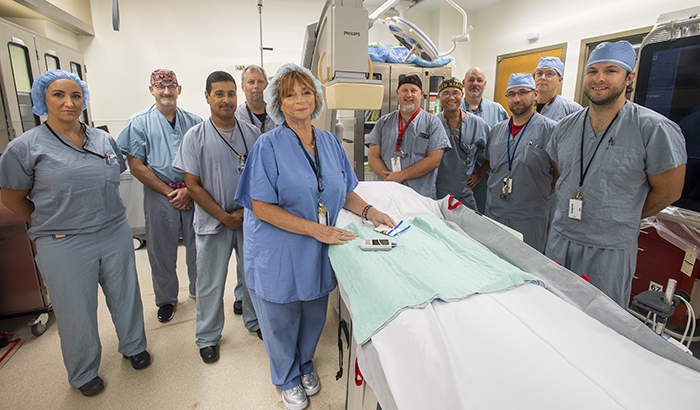
Respiratory therapist Catherine Abee displays her invention, the heat-enhanced pulse oximeter, while in the company of colleagues at the VA Pittsburgh Healthcare System. (Photo by Bill George)
August 1, 2019
By Mike Richman
VA Research Communications
"The Technology Transfer Program and TTAP...worked diligently to guide me and to make sure I’ve followed all of the steps necessary to reach the point where we are."
The idea was fresh in the mind of respiratory therapist Catherine Abee when she joined the VA Pittsburgh Healthcare System in 2008.
Abee envisioned a device that would warm an area on the body of patients being tested for the amount of oxygen in their bloodstream. The human body requires and regulates a specific balance of oxygen in the blood. Warming the measurement site, she thought, would improve blood flow and thus provide a more accurate reading. The device, a heat-enhanced pulse oximeter, could be attached to one’s fingers, forehead, foot, ears, or toes.
While working with colleagues to make the concept a reality, Abee came in contact with VA’s Technology Transfer Program, which assists researchers and other VA employees by licensing protected VA technologies to companies able to make and sell the inventions to the public. The program’s lawyers help patent VA’s inventions, which gives the owner the right to prevent others from making, selling, using, and importing the patented item or method. A U.S. patent on Abee’s invention was issued in 2017. Canadian and European patents are pending.
In 2018, Abee’s invention was adopted as one of the seven first-year products in the newly formed Technology Transfer Assistance Project (TTAP), an initiative of the Technology Transfer Program. TTAP aims to bring worthy VA discoveries closer to public use by supporting the creation of a working prototype and by consulting on pathways for commercialization. TTAP funded its main partner, the Human Engineering Research Laboratories (HERL), a large VA facility that does research, development, and testing on a myriad of technologies, to build a second-generation prototype of Abee’s device.

Dr. Rory Cooper, director of the Human Engineering Research Laboratories, displays three of the products being developed through the Technology Transfer Assistance Project (L-R): the heat-enhanced pulse oximeter, the cord caddy, and the prosthetic hook mouse. (Photo by Michael Lain)
HERL engineers have since produced a viable device that’s ready for licensing. Thus far, two companies have approached VA with an interest in licensing it, says Dr. John Kaplan, director of the Technology Transfer Program.
“Once HERL was brought on board, I met with them to discuss what I wanted the pulse oximeter to look like and what was needed to make it perfect,” Abee says. “They developed a better heat source that will plateau and maintain a warmth for hopefully eight hours. Thus, in a clinical care setting for long-term patients, clinicians know that one probe may last eight hours, so that would be one per shift. That means the product is economically sound. When HERL had a prototype ready, we met again and discussed any changes I wanted. They also adapted their equipment to keep the packaging in an enclosed environment to make sure the heat source was not activated.”
Abee is fortunate that she’s had TTAP and HERL to help bring her invention to the cusp of the marketplace. Over the years, many VA scientists, clinicians, and researchers have conceived of ideas for technologies that can help Veterans and others with their needs. But they’ve often lacked the means and guidance to convert those ideas into products with commercial potential.
That’s why TTAP was formed. The VA initiative takes bench-top or early prototype inventions and develops them—in collaboration with the inventor—so the product will be more attractive for licensing. The VA researcher is named on the patent application as the inventor, as is the case with Abee and the heat-enhanced pulse oximeter, giving more exposure to VA and its inventors. If the product is licensed to a company, VA gets royalties on the sales and possibly preferred pricing.
“Abee created a working model using commercially available components, with the idea that adding heat to the patient’s finger would thereby produce an improved blood oxygen reading,” says attorney David Marks, a VA technology transfer specialist who has worked with Abee on patenting her product. “Her original idea was the basis for the patent application. But HERL under TTAP has tried to develop a second-generation device that would be more appealing to a manufacturer to license.”

VA ear surgeon studies management of severe hearing loss in Veterans

Veteran disability payments led to fewer hospitalizations

Air Force Veteran among 10 new awardees in VA diversity, equity, and inclusion research program

VA researcher leads project to evaluate Veteran screening for malnutrition
Abee’s device is one of three first-year TTAP projects that has received a patent. The other two are the cord caddy, which prevents the tangling of a patient’s multiple IV (intravenous) lines and can be used during surgery and in other phases of a patient’s hospital stay; and the RX-1 label applicator, which attaches labels to pharmaceutical packages of various sizes and shapes faster than a person can, thus increasing efficiency in a pharmacy dispensary.
Patent applications are pending on three of the other technologies:
The other first-year TTAP project is the oxygen burn-back valve cover, a thermal fuse cover that is designed to reduce the risk of a fire in and around an oxygen gas line.
“The Technology Transfer Program and TTAP have helped me take my idea from a possibility and create a device that has been needed since pulse oximetry began in 1972,” Abee says. “Without those folks, there would be no heated pulse ox probe ready to market. They’ve worked diligently to guide me and to make sure I’ve followed all of the steps necessary to reach the point where we are. I’ve been working on this for a decade, and things have progressed amazingly over the past year.”
The thinking behind the creation of TTAP is that if a working prototype or a second- or third-generation device can be developed, instead of just something on paper, “we could have a better chance of gaining more interest from companies in licensing the technology,” Kaplan says.
“VA does a lot of research and doesn’t do too much development,” he adds. “So this is getting at more of the developmental side. It’s a team effort to prepare the product for patenting. The HERL engineers and scientists, the original inventor, and the technology transfer specialists work together to refine the invention in order to build the best prototype and submit the strongest patent application to the U.S. Patent and Trademark Office.”
U.S. government officials can issue a patent before a working prototype is created. But applying for a patent after the prototype is completed can get the inventor a stronger one that can withstand scrutiny from potential competitors, Kaplan notes.
HERL, a collaborative effort between VA Pittsburgh and the University of Pittsburgh, has a strong team of engineers and perhaps the best fabrication and standards testing facilities in VA. HERL's projects include wheelchair technologies, advanced prostheses, and other innovative systems that improve the quality of life for people with disabilities, such as lost limbs and spinal injuries. The facility is home to the VA Center for Wheelchairs and Associated Rehabilitation Engineering and is based in a state-of-the-art research and development park that includes government, academic, and private industry innovators.
HERL director Dr. Rory Cooper notes that most of the first-year TTAP products were just “back-of-the-envelope concepts” before they became part of the program.
“Now, they’re real working prototypes,” Cooper says. “You can’t really provide a Veteran an envelope, and it’s hard to license something that’s just more or less a paper concept. So we made them real.”
Cooper, who has a doctorate in electrical and computer engineering with a concentration in bioengineering, has been credited with at least 25 patents that have advanced assistive technology. He and other HERL engineers have developed each of the seven first-year TTAP technologies into a more refined prototype. He played a role in designing two of the technologies: the prosthetic hook mouse and the hand pedal. They are the only first-year TTAP innovations being manufactured at HERL.
The other five projects were invented by researchers at VA medical centers and are more “orphan” products, Cooper says, pointing out that they aren’t similar to the work that HERL normally does. “We took them in because they were what Dr. Kaplan’s group identified as areas of greatest need,” he says. Those five devices are in the pipeline to be marketed to companies via TechLink. The non-federal entity, in partnership with VA Tech Transfer and its Department of Defense (DOD) counterpart, markets VA and DOD inventions and guides businesses and entrepreneurs through the licensing process.
The development of TTAP stemmed from a visit to HERL by Kaplan to learn more about the facility and the technologies that HERL develops. He and Cooper discussed the need to build more working prototypes from research and ideas.
VA’s Office of Research and Development (ORD) first approved funding for TTAP for fiscal year 2018. ORD provides funds for TTAP that go to HERL to perform work on products that are chosen by the Technology Transfer Program.
In Kaplan’s opinion, HERL is the perfect facility to transform the technologies from concepts and designs into working prototypes.
“HERL is a unique VA resource,” he says. “It’s the only VA facility I’ve seen or heard about that has an extensive manufacturing capability across a wide range. It can do material stuff, it can do electronics, it can do a whole host of different things. In conjunction with that manufacturing capability, it has an engineering and technician staff that uses a lot of equipment and capability to build prototypes. As far as I know, no other VA facility has the manufacturing capability, the machines, the 3D printers, the ability to make electronics, like HERL. It has the ability to test devices, wheelchairs, and things like that.“
Kaplan says if VA technology transfer specialists receive an invention disclosure that includes basic information about a device that has the potential to be developed as a prototype, it can become a candidate for TTAP. Six more inventions have been proposed as second-year TTAP projects.
“We review the disclosure as a team to see if it fits for the people at HERL to build,” he says. “Normally, when the HERL engineers start building something, improvements are made to the design based on input from HERL, the inventor, and a technology transfer specialist. That team will try to perfect the design, come up with enhancements, and make it more patentable.”
As Rory Cooper sees it, the number of TTAP projects will only continue to grow. Once he and his colleagues are finished with one set, they can move onto another one, he says.
“That’s exactly what we’re doing,” Cooper says. “Those that are going to be licensed kind of graduate from our program at that point. We’ll work a little with the manufacturer, perhaps. But at that point they go on to be a commercial product, and we move onto the next thing.”
The TTAP-HERL partnership, Cooper notes, adds viability to solve the health challenges that clinicians and Veterans face.
“A lot of brilliant clinicians in VA have ideas for solutions,” he says. “They just don’t necessarily have the means to turn them into reality. What we’re doing should improve VA care and demonstrate to the public even greater value of VA, because VA will be introducing solutions that not only help Veterans but in general will help the medical community. What’s also cool is because we’re building these prototypes and trying them in VA first, that in some ways will continue to establish VA as a provider of cutting-edge care.”
VA Research Currents archives || Sign up for VA Research updates