Office of Research & Development |
 |


Black and Hispanic Veterans were twice as likely to test positive for COVID-19, even after accounting for underlying health conditions. (Photo for illustrative purposes only. ©iStock/xavierarnau)
September 23, 2020
By Erica Sprey
VA Research Communications
"Understanding what is driving these health disparities is vital."
A team led by VA researchers Dr. Amy Justice and Dr. Christopher Rentsch found that race and ethnicity is associated with a greater risk of testing positive for COVID-19, but not death within a 30-day period after hospital discharge. Justice is a clinical epidemiologist at the West Haven VA Medical Center in Connecticut and Yale University. The study was published in PLOS Medicine on Sept. 22.
The investigators analyzed the electronic health records of 5.8 million Veterans in VA care. Within that group, 254,595 people were tested for COVID-19 between Feb. 8 and July 22, 2020; of those, 16,317 tested positive and 1,057 died.
The team found a substantial excess burden of COVID-19 infection in minority communities. They identified an urgent need to develop state- and local-level strategies to reduce COVID-19 spread in minority groups.

VA center training the next generation of researchers in blood clots and inflammation

AI to Maximize Treatment for Veterans with Head and Neck Cancer

VA investigator brings diversity into autoimmune disease research

VA researcher works to improve antibiotic prescribing for Veterans
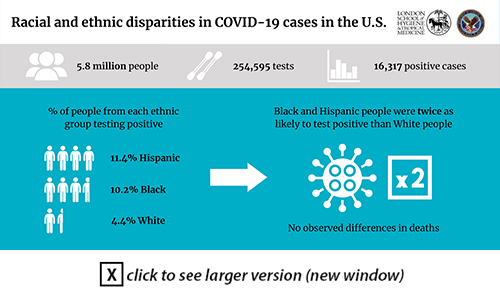
"Black and Hispanic individuals were twice as likely to test positive for COVID-19, even after accounting for underlying health conditions, other demographics, and geographic location," said lead author Dr. Christopher Rentsch, who is also an assistant professor at the London School of Hygiene and Tropical Medicine in the United Kingdom.
The study is the first to look at patterns of testing for SARS-CoV-2, wrote the authors, rather than focus just on patients who had tested positive for COVID-19 or were hospitalized because of the novel coronavirus.
The research team was composed of investigators from VA Connecticut Healthcare System, VA Palo Alto Health Care System, VA Puget Sound Health Care System, VA Tennessee Valley Healthcare System, and several other research institutions.
They found that Black and Hispanic Veterans were twice as likely to test positive for COVID-19, compared with their white counterparts. The finding held true even after the researchers accounted for underlying health conditions geographic location, and other demographic factors. However, 30-day mortality (death) rates among infected patients did not differ by race or ethnicity.
More than 250,000 individuals were tested for COVID-19 during the study period; of those, 4.4% of white Veterans were positive for COVID-19, 10.2% of Blacks were positive, and 11.4% of Hispanics were positive. The racial breakdown of study participants who tested positive was 43.9% white, 40.4% Black, and 15.7% Hispanic.
The researchers also found that Black Veterans were more likely to be tested for SARS-CoV-2 than Hispanic or white Veterans. The reason for the increased testing rate among Black Veterans was not clear.
The team was not fully able to explain the reasons behind racial disparities in COVID-19 infection. While 66% of all individuals in the study population lived in urban areas, 87% of those who tested positive were urban residents. Previous studies have found that members of minority groups are more likely to live in high-density cities or multigenerational households where the risk of COVID-19 infection is greater. They are also more likely to work in essential industries, such as public transportation, where the chance of contact with the public is increased.
VA's study on COVID-19 could help strengthen response strategies related to racial and ethnic disparities. (Photo courtesy of London School of Hygiene and Tropical Medicine.)
The researchers also found regional differences in disease incidence between Black and white Veterans. COVID-19 disparities for positive test rates in Black Veterans were highest in the Midwest region and lowest in the West. Disparities between the two groups decreased slightly over the study period. The disparity between Hispanic and white Veterans who tested positive was consistent across time, region, and outbreak patterns.
The VA study results partially replicate findings from other investigators. A retrospective cohort study in the U.S. analyzed data from an integrated health system in Louisiana. Researchers found that 76.9% of patients who were hospitalized with COVID-19 were Black, despite comprising only 31% of the patient population.
While the PLOS Medicine study found no disparity in 30-day mortality rates among those infected, for Black and Hispanic Veterans the substantial increased risk in testing positive translates to an overall excess burden of COVID-19 deaths in these minority communities.
Previous research led by the London School of Hygiene and Tropical Medicine, published in Nature, found that U.K. residents from minority backgrounds had a substantially higher risk of death from COVID-19. This U.K. study was unable to assess disparities among infected individuals due to limitations in COVID-19 testing data.
"Understanding what is driving these health disparities is vital so that strategies can be tailored to curb the disproportionate epidemics in minority communities," notes Rentsch. "Going forward, we will explore whether racial and ethnic disparities exist at other key stages in the clinical course of COVID-19."
VA Research Currents archives || Sign up for VA Research updates