Office of Research & Development |
 |
Office of Research & Development |
 |

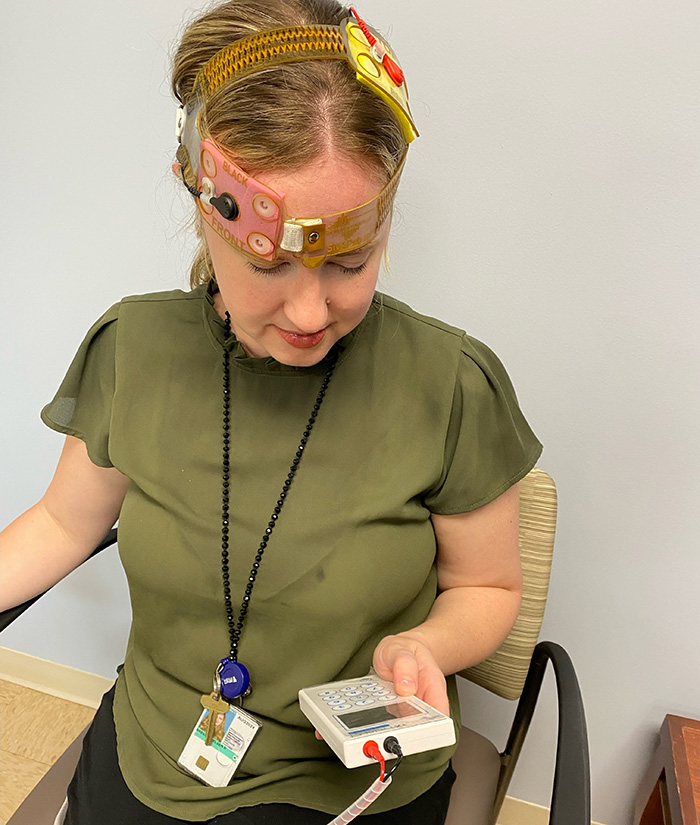
Research coordinator Chelsea Breen demonstrates how the tDCS device is used at the Ralph H. Johnson VA Medical Center in Charleston, South Carolina.
September 26, 2022
By Tristan Horrom
VA Research Communications

VA opens new research center to seek novel arthritis treatments
Injectable gel could help treat degenerative back pain

Million Veteran Program director speaks at international forum
Transcranial direct current stimulation (tDCS)—a non-invasive, painless electrical brain stimulation delivered via electrodes placed over the head—has the potential to improve chronic pain. But the treatment usually involves trips to a medical facility where the equipment is used.
In a pilot study led by Dr. Melba Hernandez-Tejada of the Ralph H. Johnson VA Medical Center in Charleston, South Carolina, VA researchers have shown that an entirely home-based transcranial stimulation treatment for chronic pain is feasible and could help Veterans with co-occurring pain and PTSD. The research team combined the treatment with a PTSD psychotherapy called prolonged exposure to treat both conditions simultaneously.
Researchers called the approach “a potentially effective path for reducing barriers to pain and PTSD care, even amid the COVID-19 pandemic.”
According to Hernandez-Tejada, who is also a researcher with the University of Texas Health Science Center at Houston, the treatment could be extremely beneficial to Veterans “because of its absence of addiction potential, ease of use, and ability to be integrated with, and perhaps enhance effects of, other treatments for comorbid conditions.”
The study was coordinated through the Ralph H. Johnson VA Medical Center in Charleston, South Carolina, and the Michael E. DeBakey VA Medical Center in Houston, with funding from the University of Texas Health Science Center at Houston.
Findings appeared in the July 9, 2022, issue of Military Medicine.
To test whether at-home tDCS could work for patients, the researchers piloted the concept with 16 Veterans with significant PTSD and pain symptoms. Lower back pain was the most common form of chronic pain in the study group.
Participants were trained to use tDCS devices from the comfort of their home using televideo, which was also used to deliver their prolonged exposure therapy. The Veterans then self-administered tDCS treatment at home under remote televideo supervision.
Participants usually did the stimulation treatment before they engaged in their prolonged exposure therapy work. Prolonged exposure is one of the most effective treatments for PTSD, according to research. The tDCS treatment began during the fourth session of prolonged exposure therapy and continued for 10 days over a two-week period.
Researchers monitored weekly symptoms of pain and PTSD. They measured both pain interference and pain intensity. Pain interference—the extent to which pain hinders a person’s engagement with physical and mental aspects of life—improved significantly after treatment.
Pain intensity did not improve as a result of the treatment. This result is not entirely unexpected, according to the researchers, and may be because the number of participants involved was quite small, as this was only a proof-of-concept trial. In addition, the prolonged exposure exercises required patients to become more active, which could exacerbate pain. The fact that stable pain levels were maintained during periods of increased activity could be considered a success, said the research team. They suggested that a larger study would be needed to track trends in pain intensity.
During the study, participants experienced significant improvements in PTSD symptoms. Although not directly treated, depression symptoms declined, and participants reported improvement in several domains of quality of life.
Finally, satisfaction with treatment was very high. Participants reported that they would recommend this combined treatment to friends, family, and other service members.
This was the first trial aimed at treating both chronic pain and PTSD to integrate evidence-based psychotherapy with a non-drug pain treatment device. Because the pilot trial proved feasible, an expanded clinical trial with more participants to test how well an at-home treatment program works seems justified, said the researchers. Along those lines, the team co-led by Hernandez-Tejada and Dr. Sheila Rauch at the Atlanta VA Healthcare System, have submitted several proposals for funding to the Department of Defense and foundations such as the Wounded Warrior Project.
Chronic pain and PTSD often occur together, particularly in Veterans. Patients with both PTSD and chronic pain often have worse outcomes for both conditions. However, the conditions are usually treated separately.
While chronic pain affects about one-third of the general population, 50% of Veterans and service members have some form of chronic pain. Managing chronic pain can be difficult because non-drug treatments are often complex and lengthy, and therefore difficult to combine with other treatments, while opioids can lead to addiction and overdose.
Many non-drug treatments for PTSD exist, such as prolonged exposure and other psychotherapies. Prolonged exposure has been demonstrated to be one of the best treatments for PTSD, and VA researchers have shown that it is effective when delivered via telehealth.
tDCS is a non-invasive treatment that has shown much promise for treating chronic pain. It involves applying low-amplitude electrical stimulation to the outside of the head. The electricity can influence neurons in the brain and alter how they respond to stimuli like pain. Hundreds of studies have shown that tDCS is safe and well-tolerated.
Brain stimulation also facilitates neuroplasticity—the brain’s ability to change and adapt—meaning it could also help the brain reorganize and adapt to treatments such as prolonged exposure for PTSD.
Recent technological advances have allowed for the remote programming of tDCS devices. In the pilot study, researchers were able to control the dose and frequency of treatment remotely, allowing for home-based self-administration.
Delivering this treatment at home could make it much more accessible to Veterans and other patients. And by combining the chronic pain and PTSD treatments, the researchers are hopeful that this approach could help improve both conditions.
VA Research Currents archives || Sign up for VA Research updates