Office of Research & Development |
 |
Office of Research & Development |
 |

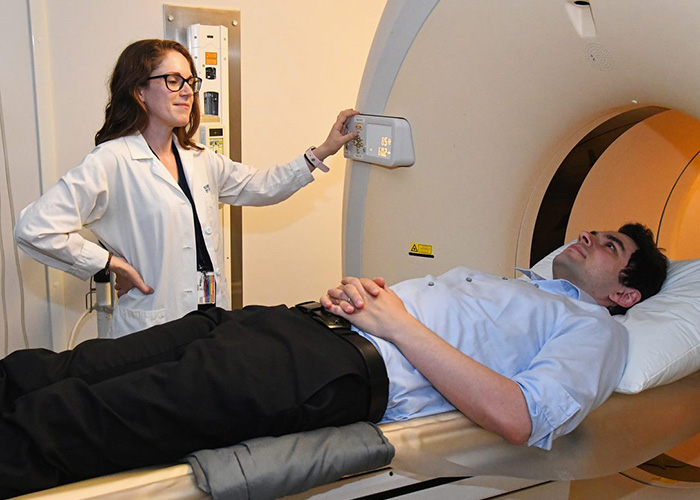
Dr. Katherine Turk, a neurologist at VA Boston, carries out a demonstration of amyloid PET imaging with Dr. Garrett Friedman, a behavioral neurology fellow at VA Boston. (Photo by Win Danielson)
September 26, 2022
By Mike Richman
VA Research Communications
"It is important to continue to develop national guidelines on the appropriate use and ordering of amyloid PET scans for behavioral neurologists."
VA-led research has found that a form of brain imaging can have a positive effect on the clinical care and management of older Veterans with Alzheimer’s disease.
In a retrospective study, clinicians at the VA Boston Healthcare System determined that using a type of positron emission tomography in Veterans with memory loss—the amyloid PET scan—can accurately diagnose or rule out Alzheimer’s disease. A follow-up study assessed the procedure’s clinical impact.
The two studies appeared in the August 2022 issue of Alzheimer’s & Dementia: Translational Research & Clinical Interventions.

Could cholesterol medicine reduce dementia risk in seniors?

VA study reveals dementia risks unique to people with African ancestry
Head trauma, PTSD may increase genetic variant's impact on Alzheimer's risk
“Our study is unique because it’s the first use of amyloid PET scans in clinical practice that showed clinical management impacts in a real-world setting,” says Dr. Katherine Turk, a neurologist at the VA Boston Healthcare System and a co-author of the research.
The first study involved 565 Veterans being treated in the Memory Disorders Clinic at VA Boston. The clinic specializes in the treatment of older patients living with cognitive decline, including Alzheimer’s disease and various types of dementia.
The clinic is also one of the few VA programs that carries out amyloid PET imaging, a minimally invasive diagnostic procedure that can spot neurologic conditions such as Alzheimer’s, one of the most common forms of dementia. PET scans use radioactive materials called radiotracers to measure changes in the brain tissue of patients with cognitive impairment that may be linked to diseases like Alzheimer’s.
Amyloid is a naturally occurring protein that accumulates in the brain of Alzheimer’s patients and forms plaques. It’s one of the most significant biomarkers found in people with Alzheimer’s and is measurable using a special form of PET called amyloid PET imaging. The technique, which is FDA-approved for diagnosing Alzheimer’s disease, is one of the most accurate ways of diagnosing the disease during life.
An alternative technique often used in clinical care is the lumbar puncture. A needle is inserted into the lower back to collect spinal fluid and measure levels of proteins involved in Alzheimer’s disease. A major disadvantage is the invasive nature of the procedure.
While amyloid PET scans are available at some facilities in the VA health care system, Turk explains that they are not typically carried out in the private sector because insurance companies and Medicare don’t reimburse for the procedure.
“We realized we’re in a special environment at VA where we’re able to obtain the amyloid PET scans that most neurologists in our field are not able to order because of insurance barriers,” says Turk, who is also an assistant professor of neurology at Boston University and a member of the university’s Alzheimer’s Disease Research Center. “We felt that use of these scans was really improving our practice and care of Veterans. We thought our VA practice environment was the perfect setting to investigate how care of Veterans is impacted by the ability to order amyloid PET scans.”
Turk led the first of two studies involving the group of 565 patients. She and her team first carried out clinical diagnostic testing to determine which patients were eligible for an amyloid PET scan. The standard clinical evaluation called for obtaining a history of the Veteran’s memory loss, performing a complete neurological exam, cognitive testing, magnetic resonance imaging (MRI) to examine brain structure, and blood work to exclude other conditions that can affect cognition.
The clinicians ordered an amyloid PET scan if they felt it would help diagnose potential Alzheimer’s disease and impact clinical management for Veterans with memory loss.
The researchers found that 197 Veterans—a little over a third of the Veterans seen in the memory clinic—received an amyloid PET scan over a three-year period, and that 98% of the scans met previously published criteria for ordering them. Turk and her colleagues were somewhat surprised that amyloid PET scans were ordered in about a third of cases. But that “just shows how useful they’ve been and that we’ve come to rely on them,” she notes.
The average age of the patients who received the PET scans was 69, compared with 76 for those who didn’t. Those who had the scan were more likely to have an initial diagnosis of Alzheimer’s disease. The scans, Turk explains, are often ordered for younger Veterans suspected of having Alzheimer’s disease.
“We know that as all of us age, amyloid builds up in the brain, and we think of the scans as having less specificity over time with age,” she says. “So that means if we find amyloid in the brain in a very old person in his or her 90s, it may just be because they’ve aged so long that they’ve started to get amyloid buildup. Many of us get that buildup with aging, but in these older patients it may not be the primary cause of their cognitive impairment.
“Alternatively,” she adds, “if we find amyloid buildup in someone who’s 60 or in their early 70s, we start to think that’s abnormal. They’re accumulating amyloid a little bit earlier than we would otherwise suspect. The incidence of Alzheimer’s is lower in a younger population. So, we think of the scan as being most useful for detecting disease in a younger population.”
Dr. Ana Laura Vives-Rodriguez, a neurologist at VA Boston and an assistant professor at Yale University in Connecticut, led the follow-up study. That paper evaluated the clinical impact of the amyloid PET scan on the 197 patients who received it in the first study.
Thirty-seven percent of those patients tested positive for Alzheimer’s. The researchers found that those rates were lower compared with other amyloid PET studies, in which positivity levels can sometimes reach as high as 50%, according to Turk.
“We concluded that Veterans are probably more clinically complex than patients in a community, non-VA setting,” she says. “For instance, a lot of Veterans have PTSD, psychiatric disorders, traumatic brain injury, and other confounding conditions. They also show signs concerning for Alzheimer’s disease. So, we would say that diagnosing these patients is challenging. Most often, their scans ended up being a way to effectively rule out Alzheimer’s.”
The researchers also determined that ordering an amyloid PET scan led to helpful changes in the patients’ care. Testing negative for Alzheimer’s was linked to longer follow-up at the Memory Disorders Clinic. “That’s because when the scan comes back negative, there’s still uncertainty as to what could be the underlying cause of the cognitive impairment,” Turk notes.
A positive amyloid PET scan was associated with less follow-up in the clinic; fewer additional diagnostic tests, such as other PET studies, an MRI, blood work, and more cognitive testing; more prescriptions for cholinesterase inhibitors, a class of medication used to treat patients with Alzheimer’s; and more research referrals.
“That’s probably because when a scan is positive, we usually have our answer,” Turk says. “We don’t need much additional investigation and testing after the scan is done and comes back positive.”
Currently, Turk and her VA Boston team are working on follow-up research using national VA data to gain a clearer picture of how often amyloid PET scans are ordered in the VA system. The researchers hope their studies will lead to greater use of amyloid PET scans in VA and potentially outside of the agency, as well, if the policies of insurance companies change.
“It will be important to continue to develop national guidelines on the appropriate use and ordering of amyloid PET scans for behavioral neurologists and other subspecialty physicians,” Turk says.
VA Research Currents archives || Sign up for VA Research updates