Office of Research & Development |
 |
Office of Research & Development |
 |
January 14, 2018
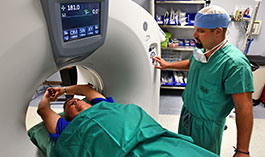
Photo by Jeff Bowen
Lung cancer is the third most common cancer among Americans and is by far the leading cause of cancer deaths in men and women. If you smoke, the best way to lower your risk of lung cancer is to quit. VA researchers played an integral role in associating smoking with lung cancer in the 1950s and 60s.
In 2011, the New England Journal of Medicine published a study of current and former smokers who were believed to be healthy. It showed that an annual screening by low-dose computed tomography (LDCT), a special kind of X-ray used to create images of your lungs, could prevent three lung cancer deaths for every 1,000 people screened for the disease. (A VA researcher in the early 1960s also pioneered the concepts that led to the development of the first computerized axial tomography [CAT] scanners, the predecessor of today’s CT scanners.)
As a result, the United States Preventive Services Task Force (USPSTF) recommends all adults aged 55 to 80 years who at one time smoked at least 30 packs of cigarettes a year and either currently smoke or have quit within the past 15 years be screened for lung cancer every year. The cost of these tests, and the number of false positive results the test generates, kept USPSTF from recommending that all Americans, or even all former smokers, receive the test.
Researchers at the VA Ann Arbor Healthcare System in Michigan played a key role in developing a tool to help patients and their health care providers weigh the risks and benefits of lung cancer screening. The online tool, called Should I Screen, was accessed more than 270,000 times between January 2015 and November 2018. It has been highlighted as effective by the National Comprehensive Cancer Network and other organizations.
In 2018, the research team completed a tool specifically for clinicians, called Lung Decision Precision, to help doctors talk with patients and their loved ones about whether a lung CT scan might be a good idea. The tool provides patient-centered recommendations based on individual risk profiles. It also offers evidence-based, personalized methods of discussing the benefits and harms of the test; allows clinicians to document their shared decision-making in electronic medical record systems; and enables them to share a printable report with patients.
VA is now funding a test of Lung Decision Precision at eight medical centers. The team is working with VA’s National Center for Health Promotion and Disease Prevention to improve the tool’s effectiveness and make it available throughout VA.
Principal investigator: Dr. Tanner J. Caverly, Center for Clinical Management Research, Ann Arbor VA Medical Center
Selected publications:
Kinsinger LS, Anderson C, Kim J, Larson M, Chan SH, King HA, Rice KL, Slatore CQ, Tanner NT, Pittman K, Monte RJ, McNeil RB, Grubber JM, Kelley MJ, Provenzale D, Datta SK, Sperber NS, Barnes LK, Abbott DH, Sims KJ, Whitley RL, Wu RR, Jackson GL. Implementation of Lung Cancer Screening in the Veterans Health Administration. JAMA Intern Med. 2017 Mar 1;177(3):399-406.
Lau YK, Caverly TJ, Cao P, Cherng ST, West M, Gaber C, Arenberg D, Maza R. Evaluation of a Personalized, Web-Based Decision Aid for Lung Cancer Screening. Am Prev Med. 2015 Dec;49(6):e125-9.
Should I Screen website
Lung Decision Precision website