Office of Research & Development |
 |


From left: Blake Henderson, acting director of the Diffusion of Excellence program, poses with Rachel Hudak and Arielle Willet at the 2019 VHA Shark Tank Competition.
January 14, 2020
By Erica Sprey
VA Research Communications
"Increasing opportunities for VHA employees to drive continuous improvement at the facility level is resulting in increased employee empowerment and engagement to solve challenges facing VA."
To improve patient outcomes, the Veterans Health Administration has taken steps to become a high-reliability organization. It is a strategy meant to drive continuous improvement in health care for Veterans.
One tenet of high reliability is welcoming innovations in patient care, especially those developed by front-line staff. Innovation has become an important part of VA's mission to care for Veterans.
VA's experiences in growing and spreading clinical innovation are described in a recent article in The Permanente Journal. Among the authors are Dr. Ryan Vega, executive director of VA's Innovation Ecosystem; Dr. Carolyn Clancy, deputy under secretary for Health for Discovery, Education and Affiliate Networks; and Blake Henderson, acting director of the VA Diffusion of Excellence program.
Launched in 2015, the Diffusion of Excellence program was created to spread promising clinical innovations across the VA health care system. Front-line VA staff have submitted 1,676 innovative practices as of publication of the article by Vega's team. Of these, 47 have been named high-impact Gold Status practices.
These Gold Status practices have been replicated 412 times in VA hospitals across the country. Estimates are that more than 100,000 Veterans have benefitted from these innovations. They range from a rapid naloxone initiative to prevent deaths from opioid overdoses, to a program called FLOW3 that aims to improve the delivery of prosthetic services to Veterans.
"Diffusion provides a sustainable, established platform and process for engaging groups at all levels," wrote the authors. "Increasing opportunities for VHA employees to drive continuous improvement at the facility level is resulting in increased employee empowerment and engagement to solve challenges facing VA."
Translating the most promising clinical research into treatments for patients has typically been a slow process. It can take many years before new technologies or clinical breakthroughs are routinely available to patients.
There are many factors that can delay innovation across a health system. The complexity of the solution, the cost for implementation, limited resources, and lack of innovation champions can all slow down adoption of innovation.
VA has created a structured approach to address these challenges and to support the replication of promising clinical solutions across the enterprise. The "Diffusion Model" has five steps: identifying promising clinical innovations; finding innovation champions; adapting and replicating Gold Status practices; measuring real-world impact; and scaling and spreading best practices.

VA in new research agreement with National Institute of Allergy and Infectious Diseases

Spreading innovation across VA health care
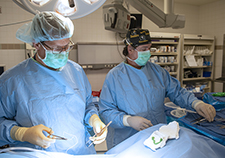
Study raises new warnings about frail surgery patients
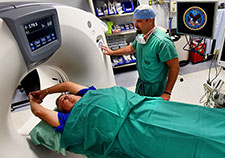
Smokers hazy on actual benefits of lung cancer screenings
It is usual practice for hospital administrators to establish clinical policies for medical staff. However, front-line staff often have a unique understanding of clinical care, as they are closest to patients and their families.
VA's Diffusion of Excellence program seeks to take advantage of that unique perspective. It hosts an annual competition modeled after the TV show “Shark Tank." Employees are invited to submit their ideas for innovations that will improve health care for Veterans. The submissions must have already demonstrated improvements at local VA facilities.
A team of experts review the submissions, looking for demonstrated value, the ability to be replicated in other facilities, and alignment with VA priorities. Approximately 100 semi-finalists are then rated on a 10-point scale by researchers from the VA Quality Enhancement Research Initiative (QUERI). The team is looking for clinical soundness, potential for impact, and feasibility within VA.
Once review is completed, about 20 finalists are invited to "pitch" their solutions during a live Shark Tank. VA medical centers and Veterans Integrated Service Networks (VISNs)—the Sharks—bid for the chance to implement practices at their facilities. A bid might consist of staffing, funding for equipment, or facility space.
At the conclusion of the finalists' presentations, a governance board composed of senior VHA leaders chooses the best innovations for further implementation within the VA health system. These "winners" are called Gold Status practices. The practices are paired with one to three implementing facilities—the sharks who have submitted a winning bid.
The winning innovations from the 2019 VA Shark Tank address a gamut of Veteran needs. They include a boot camp to help Veterans with Parkinson's disease reduce falls; a pre-surgical screening program for frailty measures; and a program that will involve VA police officers to support mental health outreach for Veterans.
HAPPEN is a successful VA innovation that was promoted to Gold Status in 2016. The acronym stands for "Hospital Acquired Pneumonia Prevention by Engaging Nurses to provide oral care."
Its creator, Dr. Shannon Munro, is a nurse-researcher at the Salem VA Medical Center in Virginia. Using data collected from a pilot program, Munro and her team published research that demonstrated the effectiveness of consistent oral hygiene in preventing non-ventilator associated hospital-acquired pneumonia (NV-HAP).
Hospital-acquired pneumonia is a serious illness that kills up to a third of affected patients in the U.S. It is one of the most common hospital-acquired illnesses that patients develop in hospitals or long-term care facilities.
NV-HAP accounts for more than 60% of all cases of hospital-acquired pneumonia. This is due, in part, to a lack of formal nursing protocols to assist patients with oral care in hospitals or long-term care facilities. In contrast, there are well-established protocols to help prevent ventilator-associated pneumonia.
Studies have shown that brushing patients' teeth two to four times a day can reduce their risk of developing NV-HAP by 40% to 60%. During sleep patients can aspirate (swallow) the bacteria in their mouths into their lungs, potentially causing pneumonia. Brushing patients' teeth and cleaning dentures on a regular basis is a low-cost intervention that has saved lives.
Munro and her team initiated a pilot program at the Salem VA's Community Living Center (CLC) to engage staff to brush Veterans' teeth at least twice a day. The pilot reduced the incidence of NV-HAP at the Salem CLC from 105 to 8.3 cases per 1,000 patient days, representing a 92% reduction in disease in the first year. Over 36 months, the Salem CLC pilot intervention saved an estimated $5.4 million and 24 Veteran lives.
Once HAPPEN was promoted to a Gold Status practice in 2016, it was then implemented in eight VA medical facilities across North Carolina, Texas, and Virginia. To date, the practice has been adopted by 54 VA hospitals.
Not all Gold Status practices are disseminated across the VA health system. After a six-month facilitated replication period at selected VA health care sites, the projects are evaluated for further implementation. Leadership considers factors like need, ease of replication, and cost of implementation.
Based on the success of its initial implementation, HAPPEN was chosen for national dissemination across the VA health care system. Munro has been designated National HAPPEN Implementation Lead and is spearheading the implementation of the Gold Status practice across the country.
HAPPEN is one example of a high-impact innovation, according to the study authors. Munro and her team took a simple concept—one that is relatively easy to implement—and turned it into high-value care that has saved the lives of many Veterans by avoiding hospital-acquired pneumonia.
"The shortest task, tooth brushing, was considered a low priority by many before we started this journey," Munro told VA public affairs officer Brett Robbins. "Now we are seeing Veterans and staff paying more attention to this life-saving, two-minute-per-shift intervention. Health care providers and family members play an important role in making sure that oral care is provided consistently for our Veterans during their hospital stay."
VA Research Currents archives || Sign up for VA Research updates