Office of Research & Development |
 |

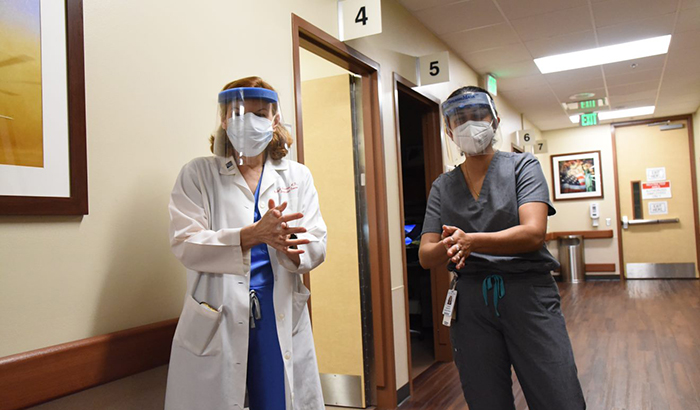
Drs. Barbara Trautner (left) and Lavannya Pandit are leading a clinical trial at the Houston VA, as part of a larger network of study sites, examining the anti-inflammatory drug tocilizumab for COVID-19. (Photo by Regit Sasser)
July 27, 2020
Mike Richman
VA Research Communications
"The Veterans we are enrolling in this study are eager to join the fight against COVID-19. "
A drug often used to treat rheumatoid arthritis by lowering inflammation levels is the focus of a new clinical trial on COVID-19 patients with severe pneumonia.
The VA hospitals in Houston and Miami are among the nearly 70 medical sites participating in the international double-blind study on the drug tocilizumab, or TCZ (trade name Actemra). About 40 of the sites are currently active.
“COVID-19 is known to cause extensive damage in the lungs, often leading to difficulty breathing and eventually pneumonia,” says Dr. Lavannya Pandit, a pulmonologist and critical care physician at the Michael E. DeBakey VA Medical Center in Houston.“Pneumonia triggers a hyperimmune response that can be more detrimental to some patients than the original infection.”
Pandit and Dr. Barbara Trautner, an infectious disease expert, are the co-investigators of the study at the Houston VA. Both clinicians are affiliated with the Baylor College of Medicine in Houston, which is also participating in the trial. Dr. Paola Lichtenberger, an infectious disease specialist, is the lead investigator at the Miami VA Healthcare System.

VA researchers using AI to decide best treatment for rectal cancer

VA center training the next generation of researchers in blood clots and inflammation

AI to Maximize Treatment for Veterans with Head and Neck Cancer

VA researcher works to improve antibiotic prescribing for Veterans
TCZ is in a class of drugs that reduce the strength of the body’s immune system. An overactive immune system is often as harmful as one that stops working, with the potential to lead to many types of autoimmune diseases, a condition in which one’s immune system mistakenly attacks the body. Hyperactive immune responses prevent the body from telling the difference between a person’s healthy cells and invader cells.
TCZ is often used to treat rheumatoid arthritis, a chronic condition characterized by joint inflammation, and systemic juvenile idiopathic arthritis, a severe form of arthritis in children. The drug has the potential to block interleukin-6 (IL-6), a chemical that plays a key role in the body’s immune response and is involved in the development of many diseases. They include autoimmune diseases, prostate cancer, and multiple myeloma, which causes cancer cells to accumulate in bone marrow and crowd out healthy blood cells.
In June, the U.S. Food and Drug Administration (FDA) gave emergency use approval to the makers of TCZ for an IL-6 test to help treat severe inflammatory response in COVID-19 patients.
Eligible participants in the TCZ trial include hospitalized patients diagnosed with severe COVID-19 pneumonia that is marked by dangerously low blood oxygen levels. Severe pneumonia levels are confirmed by a PCR test, the most common type of test for coronavirus, and chest imaging.Nearly 400 people at medical centers in the United States, Africa, and Latin America are participating in the trial, with two-thirds in the TCZ group. They are receiving an injection of TCZ on day one, with the rest getting placebo and standard of care. TCZ has a half-life of two to three weeks.
Patients on ventilators are not eligible to enroll. “We enroll patients who are able to breathe on their own,” Trautner says. “The goal is to prevent the need for a ventilator.”
The trial reached its enrollment target in mid-July. The Houston VA enrolled 16 Veterans in their late-30s to their late-70s. The two Veterans who are enrolled at the Miami VA are 69 and 48 years old. All participants are being monitored for 28 days for their response to the treatment, including disease progression, length of hospitalization, and the need for critical care and other supportive treatments. The primary outcome measurement is the number of participants who will require mechanical ventilation by day 28, with the death rate among the secondary measurements.
The participants in the placebo group will not be getting TCZ at the end of the trial.
“The hypothesis is that TCZ can prevent the inflammatory response in COVID pneumonia that leads to uncontrolled inflammation and respiratory failure,” Trautner says. “Therefore, the drug must be given while the patient is newly hospitalized with COVID pneumonia.”
At the Houston VA, Trautner points out, “first contact from the sponsor [Genetech, Inc.] to full approval took only 16 days”—an impressively short period of time for a clinical trial start-up. She credits an array of partners in the effort, including the VA Office of Research and Development, the Baylor College of Medicine, and the Houston VA Research and Education Foundation (HVAREF).
HVAREF is one of a network of nonprofits affiliated with VA medical centers nationwide to help support research. The umbrella organization for these nonprofits is known as NAVREF. Earlier this year, in collaboration with VA, NAVREF launched the Partnered Research Program to make it easier and faster for VA sites to launch industry-sponsored trials. The program is an outgrowth of the larger Access to Clinical Trials (ACT) for Veterans initiative launched by VA a few years ago.
Because of clinical trials like the new TCZ study, Trautner says, the treatments that are offered for COVID-19 in three months will differ considerably from what is now available. She notes that randomized controlled trials have generated evidence that the antiviral drug remdesivir and dexamethasone, a steroid, may help treat severe cases of COVID-19. Remdesivir is FDA-approved to treat COVID-19 pneumonia. But the data on dexamethasone, which has not been approved to treat COVID-19, are preliminary.
Scientists found remdesivir to be superior to placebo in shortening recovery time in hospitalized patients with COVID-19 and lower respiratory tract infection. Dexamethasone resulted in lower 28-day death rates among COVID-19 patients who received ventilation or oxygen alone at randomization, but not among those receiving no respiratory support. At the Houston VA, Trautner notes, most Veterans hospitalized with COVID-19 pneumonia receive both remdesivir and dexamethasone, which is consistent with VA and national treatment guidelines.
“Our trial will similarly advance knowledge about whether tocilizumab should be added to the treatment regimen,” Trautner says. “Hundreds of other randomized controlled trials are going on worldwide. Collectively, these will yield level-one evidence that will change care standards.
“The Veterans we are enrolling in this study are eager to join the fight against COVID-19,” she adds, “and we are happy to provide them this opportunity and do our part. VA offers cutting-edge treatments and top-quality care for Veterans with COVID-19. Participating in this clinical trial allows our Veterans the opportunity to contribute to scientific progress.”
VA Research Currents archives || Sign up for VA Research updates