Office of Research & Development |
 |


Donald Salganik, who served in the Air Force during the Korean War, proceeds through an obstacle course that is part of the "multimodal balance intervention" being studied by Baltimore VA researchers. With him is study coordinator Lydia Paden. (Photo by Mitch Mirkin)
November 28, 2017
By Mitch Mirkin
VA Research Communications
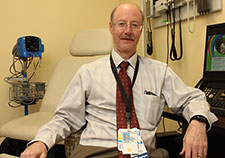
Dr. Les Katzel, a geriatrician, studies the effects of exercise and weight loss on the health and function of older adults. He is with the Baltimore VA Medical Center and the University of Maryland. (Photo by Mitch Mirkin)
If you’re up in years and don’t get around so well anymore, take heart from a group of seniors at the Baltimore VA Medical Center.
These older Veterans are making strides—literally—in their ability to move about, stay balanced, prevent falls—and get up from a fall if they do have one.
They’re part of a research program that has been evolving over the past 15 to 20 years. It’s based at the Geriatric Research, Education, and Clinical Center at the Baltimore VA Medical Center—one of 20 such centers throughout the VA system. Support comes from VA, the National Institute on Aging, and other sources.
Much of the research takes place at an annex a few blocks from the hospital in downtown Baltimore. Visit here on a weekday morning and you’ll find a group of aging Veterans working out on machines and doing a variety of movement drills, under the watchful eye of exercise physiologists.
But it’s not your typical neighborhood gym, or even your standard medically supervised exercise program. There’s rigorous science driving the action. The researchers want to learn the safest and most effective ways to build, restore, and preserve mobility—and thus independence—for these men and women who wore the uniform, some from as far back as the Korean or even World War II era.
Talking about his team’s newest study, Dr. Les Katzel says: “The age range for the study is 60 to the 90s. There’s no upper age limit. We believe everybody should be exercising. And it’s never too late to try and prevent falls.”
"It's important to mix it up, and to have fun. Otherwise, it gets repetitive."
The Veterans targeted in the new study not only have mobility problems, they are also considered obese. They have a body-mass index, or BMI, of 30 or higher. That translates, roughly, into 30 extra pounds or more. The obesity prevalence among VA patients overall tops 40 percent, according to a 2017 study.
To the casual observer, some of the participants in the GRECC study barely look overweight, let alone obese. Katzel asserts that “given the marked secular [general] increase in obesity over the past two decades, we are so used to seeing obese individuals that in some ways it has become the new normal, and appearances are deceiving.”
And it’s not just the extra pounds. For most of the group, it’s also low muscle mass. The combination, which Katzel calls a “double whammy,” is known as sarcopenic obesity.
“We have to improve their strength and function, and help them get some of the weight off, while preserving muscle mass,” explains Katzel.

Army Veteran Gary Lucas navigates a hurdle exercise with the help of study coordinator Lydia Paden. (Photo by Mitch Mirkin)
Most of the Vets in the study are coping with other health challenges too: diabetes, high blood pressure, clogged arteries, depression.
“On average the people coming into the program have 10 to 15 active medical problems,” notes Katzel. “They are taking 15, as many as 30 medications a day.”
Many have begun using assistive devices to get around, such as walkers or canes. Some have been prescribed the devices but resist using them, thus raising their risk of falls.
The research team is undaunted. Katzel says most past studies on geriatric mobility have excluded this population. His group is seeking them out. Some of the seniors are on the verge of being homebound, and even getting to the annex three times a week for the year-long study is a challenge. Notwithstanding the logistics hurdles, the study aims to enroll up to 120 Veterans in all.
Katzel says the GRECC exercise program, over time, has worked with increasingly more challenging populations of Vets, in terms of their health issues.
“When we first started years ago, with a GRECC clinical demonstration project, we tended to focus on really healthy older adults”—athletes, essentially. (One extreme example: His team has published findings on a runner they followed for several years, and who by age 91 had completed an amazing 627 marathons and 117 ultra-marathons.)
“Then, over the years,” continues Katzel, “we focused on certain diseases and their impact on mobility—stroke, peripheral arterial disease, heart failure, Parkinson’s, and HIV. In this population [enrolled in the new study], along with the mobility problems and obesity, they have a lot of orthopedic issues.”
So how do you go about boosting mobility in such a challenging population?
The researchers use what they call a “multimodal balance intervention,” or MMBI. The emphasis is on improving balance and side-to-side movement, and building strength in the legs and core, through a variety of specially designed exercises.
“One thing we’ve recognized over the years,” says Katzel, “is that if you put someone on a treadmill or a bike, that’s good, it’s certainly better than nothing, but it doesn’t really help them in a lot of other areas, like lateral movement. It’s also clear that these folks have markedly decreased strength in their legs. They have particular difficulty getting out of a chair, for instance. The multimodal program combines having lateral movement, strength training, balance exercise, and some other things to address these multiple deficits.”
Katzel’s colleague Dr. Odessa Addison, a physical therapist by training, adds, “MMBI tries to get them to move in all planes of movement, to use all their muscles.”
Half the enrollees are also receiving weekly nutrition sessions and individualized diet plans, with the goal of helping them lose 10 percent of their baseline weight. (See sidebar.) The researchers are comparing this group to the exercise-only group as the study progresses. They will look at outcome measures such as distance walked in six minutes, aerobic endurance, body composition, quality of life, and ability to perform activities of daily living.

Roger Bergeron, who served in the Navy, works his hip abductors as exercise physiologist Katie Dondero adjusts the machine settings. (Photo by Mitch Mirkin)
After a medical check-in at each session, the participants get moving.
“Step to the side, bounce and catch! Step to the side, bounce and catch!” That’s the instruction from exercise physiologist Katie Dondero as she demonstrates the motion at one of a handful of stations in the MMBI classroom session. The Vets follow suit, bouncing a blue ball on the floor and catching it, and continuing the drill as they shift left and right.
They move from station to station during the 30-minute session, dance music pumping in the background.
At one corner, they step over a series of yellow mini hurdles.
“This involves step planning,” explains study coordinator and exercise physiologist Lydia Paden. "We want to make sure they pick up their feet and watch out for the obstacles in front of them.”
Her colleague Jeff Beans, also an exercise physiologist, points out that standing on one leg, even for a second, can be physically difficult—and a bit scary—as people age. “One of the challenges for older adults is their ability to move through the normal range of motion for walking and do it safely. You watch an older adult move, you’ll see the stride get shorter and choppier because they’re uncomfortable with that single leg they’ve got to stand on for part of the stride.”
At another station, the Vets grasp a wall-mounted balance bar with one hand and do forward lunges. At the next, they bounce a ball off the pale-yellow brick wall, aiming for an X marked at just above head level. Another station has them getting up out of a chair, with a catch: There’s a mat under their feet that gets higher as they progress through the program.
“Getting up out of a chair becomes difficult for many older people,” explains Katzel. “Those are the types of deficits we address. We measure how many chair rises they can do in 30 seconds. We increase the challenge over time by having them stand up onto cushions of different heights.”
After the classroom portion, the group moves into the large gym area. Here, some do leg lifts while others use a pulley machine, raising one leg at a time out to the side to work a group of muscles called the hip abductors.
Addison found this exercise to be one of the keys to fall prevention in her previous studies.
“When we looked at the differences in muscle strength between fallers and non-fallers, the muscles that were most impaired were the hip abductors.”

One obstacle-course exercise has the Veterans walk over an uneven pile of mats that simulates risks in the home—such as changes in floor textures and heights, or area rugs—that could present fall risks. (Photo by Mitch Mirkin)
The finale of the morning session is the obstacle course. At one end of the oval track ringing the gym, a row of small orange cones has been set up. The Veterans have to tap each with their toes as they move sideways.
They move on to a drill resembling the hurdle exercise they did in the classroom—only here, they do it on the track.
“Whatever skills they’re working on in a static environment in the MMBI class, we’re moving toward a dynamic setting,” explains Beans. “People don’t fall when they’re sitting or standing there—they fall when they’re moving. So what we’ve created here is a progressively more challenging obstacle course.”
Addison sums up the program as follows: “The whole idea behind MMBI is that we train the movements we want, we train the muscles to be able to do those movements, and then we put it all together on the obstacle course.”
The obstacle course also includes a set-up the team calls “London Bridges”—a series of platforms that simulates steps at home, or perhaps a curb on the street. By practicing here, with no cars whizzing by, the seniors build confidence to navigate similar settings outdoors.
The course ends with a bunch of blue rubber mats piled on the track in a staggered fashion. The idea here is to simulate changes in floor textures and heights—for example, going from a hardwood floor to a carpet. This is a frequent culprit in geriatric falls. It also trains the seniors to avoid tripping on a blanket or rug at home.
“It’s all directed at their specific limitations and challenges,” stresses Katzel.
Many of the participants have in fact fallen in the past—some are referred to the study by VA physical therapists who worked with them in rehab. And it’s not unlikely that some will fall again, even with the gains they made in the study. “One of the things we do in the program is actually teach them how to get up off the floor,” notes Addison. “If they’ve had a fall in the past, that’s usually a big fear.”
The hope is that after the year-long study ends, the Veterans will continue to work out. The team trains the seniors on a home program. For those who want to maintain the group comradery—and some supervision—one option is Gerofit, a supervised exercise program that was developed at the Durham VA Medical Center in the 1980s. Today it’s available at VA sites nationwide, including Baltimore.
It includes some elements found in MMBI, but offers a wider palette of options, ranging from tai chi and line dancing to stair climbers and weight machines. The goal is a personalized program tailored to individual needs, but in a fun group atmosphere.
Katzel says the Baltimore Gerofit team, as part of a VA-wide initiative funded by the agency’s Office of Rural Health, has used VA’s telehealth system to “beam” tai chi instruction and other exercise classes to Veterans in remote locations, including other states. According to research, tai chi can cut the fall risk among older people by about half.
For his part, Katzel says he would like to see as many Vets as possible make the transition to Gerofit.
“It’s difficult to measure, but there’s clearly a social benefit from people coming here. There’s emotional support.”
Also crucial, says Katzel, is the variety and creativity of the activities in programs like MMBI or Gerofit.
“It’s important to mix it up, and to have fun. Otherwise, it gets repetitive.”
Study participant Donald Salganik, 86, who served in the Air Force on a B-36 “Peacemaker” bomber during the Korean War, clearly enjoys the banter with his fellow Veterans as they sweat through the morning workout. But for him, the biggest benefit is perhaps even more basic. His favorite part, he says, is simply “just moving. I wasn’t moving much before coming here.”
Fewer calories in, more calories out.
That’s the basic approach being applied in the nutrition arm of the multimodal balance study.
“It’s pretty standard in research,” notes dietician Dr. Elizabeth Parker, part of the study team. “Most studies will use a reduced calorie diet for weight loss.”
The protocol also aims to raise protein intake, to maintain muscle mass. The extra protein can come from whatever healthy foods the participants prefer: more fish or cheese, for example.
“We’re trying to space it out so you get about 30 grams per meal,” says Parker. “With weight loss, a lot of people tend to lose not just fat, but muscle as well. We’re trying to minimize the muscle loss while maximizing the fat loss.”
The strategy is backed by studies such as one that came out earlier this year in the Journal of the American Geriatrics Society. Researchers on the Health ABC Study tracked nearly 2,000 older adults and found that those who ate the least protein were almost twice as likely to have trouble walking a quarter mile or climbing 10 stairs, compared with the group that consumed the most protein. The study wasn’t a controlled trial designed to show cause and effect, but it does support the notion that higher protein intake helps preserve muscle mass and, therefore, mobility.
One possible limitation of the diet phase of the study, like most research of this kind, is that it relies on self-reports from the Veterans about what they are eating. They might not be fully forthcoming, for example, about snacks and sweets.
But rather than have the Veterans simply keep a written log, the study is using a computer-aided system to collect the information. It’s based on something developed by researchers at the USDA called the Automated Multiple-Pass Method. It offers cues to help the study participants remember and describe what they ate and drank, and is thought to result in more accurate food logs.
Besides, as Veteran Will Simister pointed out as he met with Parker to go over his diet plan, “it would be self-sabotage” to intentionally fudge the reports. He served as a corpsman in the military and went on to be a physician assistant.
Parker emphasizes to all the participants that they are not being judged on their food habits.
“We’re just using this as a tool to figure out what you’re currently eating and how we can modify it to make it better.”
VA Research Currents archives || Sign up for VA Research updates