Office of Research & Development |
 |


Drs. Regina McGlinchey and William Milberg, directors of VA’s Translational Research Center for TBI and Stress Disorders (TRACTS), review MRIs. (Photo by Frank Curran)
March 31, 2020
Mike Richman
VA Research Communications
Chris Riga knew something wasn’t right.
While standing for a few minutes at a ceremony in Afghanistan in 2005, the Army Ranger suddenly felt like he was losing his balance. “It almost felt like I had vertigo or something like that,” he says. “I was unstable and had to lean on something.”
Riga was exposed to a series of roadside blasts while serving in Afghanistan and Iraq from 2001 to 2014. He wasn’t diagnosed with brain trauma until leaving the service. But just being in the vicinity of explosions has left him with challenges today. In addition to an unsteady gait that causes an occasional loss of balance, he experiences short-term memory loss.
“When I get that vertigo-like feeling, I’ll usually hold onto or lean on something,” says Riga, who is 55 years old. “The short-term memory issues are easily solved by writing things down or taking notes. I’ve always used stickies as reminders. I keep them all over my desk and put them in my wallet and pockets. One of the greatest inventions is the smart phone. You can set alerts on the phone as reminders.”

Former Army Ranger Chris Riga was exposed to a series of roadside blasts while serving in Afghanistan and Iraq from 2001 to 2014. (Photo courtesy of C. Riga)
Struggles with balance and memory are potential symptoms of mild traumatic brain injury (mild TBI), the focus of the VA program in which Riga is enrolled: The Translational Research Center for TBI and Stress Disorders (TRACTS). The initiative is aimed at understanding the long-term impact of TBI, the signature injury from the conflicts in Iraq and Afghanistan, on the physical and mental health of post-9-11 Veterans. Improved medical care has enabled many troops to survive with brain injuries, hence the urgent need for advancements in research efforts and treatment options.
Most TBI injuries are considered mild. But even mild TBI, also known as a concussion, can involve headaches and long-term effects on thinking ability, sleep, mood, focus, balance, and memory.
TRACTS, based at the VA Boston Healthcare System, is carrying out one of the most comprehensive VA studies on blast injuries on post-9-11 Veterans. Since the program was launched more than a decade ago, about 850 Veterans have participated in its flagship project: a prospective long-term cohort study that includes an assessment of psychological and brain trauma. Of the 850 Vets who have completed the assessment once, nearly 500 have returned for a second time and close to 70 a third time, helping researchers learn if the participants have experienced changes in brain structure and function as they age.
"We can look at a person's trajectory across his or her life span, as opposed to doing group analyses where you compare one big group of people to another."
The average age of the Veterans who have been in the program is 32, and the age range for the first evaluation has been 18 to 65.
“It’s very special that we’ve had so many people return,” says Dr. Regina McGlinchey, the director of TRACTS. “We conduct this as an aging study, so the benefit of having longitudinal data is that we can look at a person’s trajectory across his or her life span, as opposed to doing group analyses where you compare one big group of people to another. Our approach is very different and much more powerful.
“TBI is a risk factor for Alzheimer’s disease and other types of dementia, but the impact doesn’t have to be that drastic to affect a person’s life,” she adds. “We can see declines in other cognitive functions in young people, such as memory, that we wouldn’t ordinarily see until someone is much older. We call this accelerated cognitive aging.”

Blood pressure drug could prevent posttraumatic headaches

Five ways the Million Veteran Program is transforming our understanding of Veteran health

Traumatic brain injury carries risk for cardiovascular disease in post-9/11 Veterans
Head trauma, PTSD may increase genetic variant's impact on Alzheimer's risk
The patients in TRACTS have been evaluated at the Boston VA and the Michael E. DeBakey VA Medical Center in Houston. About two-thirds of the Veterans have undergone at least one assessment in Boston. The program is eligible for a five-year funding renewal in 2023.
Data from the TRACTS cohort study have been the basis for more than 100 published papers that explore the impact of TBI and other conditions, such as PTSD, depression, and substance abuse (see sidebar). TRACTS has 35 primary researchers, plus other investigators who are affiliated with the program.
The TRACTS assessment is based on a 10-hour battery of tests that was compiled by the TRACTS team at the Boston VA. Psychiatrists and psychologists interview Veterans about their exposure to blasts and traumatic events and to determine, for example, if they also have a history of PTSD, depression, or substance abuse. The clinicians also test the Veterans’ cognitive skills and administer MRI (magnetic resonance imaging) brain scans. Plus, the patients provide a blood sample that is evaluated for standard measures, such as glucose and cholesterol, as well as genetic and methylation analysis. Methylation can change the activity of a DNA segment without changing the sequence.
One of the tests in the 10-hour battery is a lifetime assessment of head injuries. It allows researchers to determine which Veterans were exposed to blasts, how many explosions they were exposed to, and their distance at the time from the blasts.
“We can also determine whether blast exposure resulted in a TBI doing a very careful re-creation with the patients about whether they had concussion-like symptoms at the time of the blast,” says McGlinchey, who is also a professor of psychiatry at Harvard Medical School. “For example, one can have a loss of consciousness, memory impairment, or a feeling of confusion or of having your bell rung, so to speak, at the time of the blast. We also look at pre-military service for things like childhood head injuries and at whether the Veterans sustained injuries after separating from the service. In addition, we do a lifetime comprehensive assessment of PTSD, and whether there are anxiety disorders, depression, or substance use.”
McGlinchey and the co-director of TRACTS, Dr. Bill Milberg, are very interested in studying the potential brain trauma that emerges from being in the vicinity of a blast but does not necessarily involve a concussion, as is the case with Chris Riga.
“When we look at brains, one of the consistent findings is that blast exposure actually has a larger effect on the brain than the concussion itself,” says Milberg, who is also a professor of psychiatry at Harvard Medical School. “We’ve accumulated enough data to see people who’ve been exposed to a large blast or a close blast who really don’t seem to suffer a concussion at the time of the blast. Yet, they have enduring changes in their brain. Those enduring changes are both structural and functional. That’s very important. If they’ve had blast exposure, they’re also more likely to have long-term consequences in their cognitive functions, as well, whereas we don’t see that from concussion alone.”
If studying the issue of proximity to blasts is not “the most important aspect of TRACTS, it’s a close second,” says Riga, who commanded a special operations task force in Afghanistan that included members from the Army, Navy, and Marines.
“I say that because so many Veterans and active-duty personnel have suffered or are still suffering from some type of trauma just by being near locations,” he says. “I’ll give an example. To no one’s fault, for years we didn’t understand the effects of things like anti-tank weapons, whether you fired it yourself or were in proximity of it. We’ve learned that certain weapon systems cause great back blast and blast effects near and around. That not only affects the firer, but those around him, too. Things like that are being done daily in training, never mind in combat. It’s not just the anti-tank weapons. It’s also soldiers who are undergoing close-quarter battle-type training.”
The Defense and Veterans Brain Injury Center reported nearly 414,000 TBIs among U.S. service members worldwide between 2000 and late 2019.
Mild TBI is usually more difficult to identify than severe TBI. That’s because there may be no observable head injury, even on imaging, and because some of the symptoms resemble those from other health conditions that may also emanate from combat trauma, such as PTSD.
Through TRACTS, McGlinchey and Milberg are also seeking to better comprehend the combinations of diagnoses that can accompany brain trauma. Most Iraq and Afghanistan Vets have on average three different diagnoses, the two TRACTS leaders note. They hope the researchers who analyze the TRACTS data can identify combinations of conditions that seem to predict poor outcome.
“We’re trying to understand which combinations of diagnoses and bodily systems are feeling the impact that can give us a clue as to who’s going to be okay in the long run versus who’s going to need help in the short and long term,” McGlinchey says. “You can’t really look at these things in isolation as if they’re not influencing one another. For instance, researchers have found that mild TBI, PTSD, and depression, a combination called the `deployment trauma phenotype,’ are often seen together and are associated with particularly poor long-term functional problems.”
Milberg: “Who are the greatest risks for increasing medical and psychological challenges? That’s what we’re trying to figure out.”
Researchers at TRACTS have published several papers showing that a concussion that occurs without accompanying psychiatric diagnoses and other histories, such as PTSD or depression, is a “very different phenomenon,” Milberg says, than a concussion that co-occurs with such diagnoses. “Psychiatric problems are much more severe in the context of a person who’s had a head injury,” he explains. “It’s almost paradoxical because if you see the people who only have concussions, their outcomes are pretty good. But the people who have concussions and other diagnoses are much worse off than other people with those diagnoses who don’t have concussions.”
The ultimate aim of TRACTS and other research efforts on TBI is to help heal Veterans. Researchers want to produce psychological and biological findings that lead to new diagnostic techniques and treatments. Currently, TRACTS researchers are pursuing a series of studies that examine therapies, including medication, cognitive behavioral therapy, and brain stimulation. In the largest study, Dr. Catherine Fortier of the Boston VA is leading research on the effectiveness of a program called “STEP-Home,” which is a workshop open to all Veterans who are having trouble reintegrating into civilian life following deployment.
TRACTS isn’t the only VA endeavor with the ambitious goal of unlocking the mysteries of traumatic brain injury. The initiative and its long-term cohort study predated the joint DoD-VA Long-term Impact of Military Relevant Brain Injury Consortium (LIMBIC), which began in 2013 as the Chronic Effects of Neurotrauma Consortium (CENC).
LIMBIC, based at the Hunter Holes McGuire VA Medical Center and Virginia Commonwealth University in Richmond, Virginia, features the world’s largest research cohort dedicated to the study of mild TBI. The five-year program is centered on two elements. One is a long-term study of 3,000 to 5,000 Veterans and service members from U.S. conflicts and wars dating back to World War II, 80% of whom will have had at least one mild TBI. The other 20% of the participants, who also experienced combat but are concussion-free, serve as the control group. One goal of LIMBIC: By comparing the two groups, the researchers hope to learn if just being a service member in combat is contributing to neurological problems, such as dementia and Parkinson’s disease, even absent a history of traumatic brain injury.
The other core element is an epidemiological database of military and VA health records, disability assessments, and all other administrative information on more than 2 million Vets and service members from U.S. conflicts and wars. Only a small percentage of that cohort had combat-induced brain injuries.
For his part, Chris Riga is working to recruit Veterans to TRACTS. He’s twice undergone the program’s 10-hour battery of tests and is thrilled to be a part of an initiative that helps Veterans who are seeking solutions to their brain injuries.
“What a great program this is,” he says. “I know there are very few programs doing the same type of research. It’s phenomenal that many Vets turn out to do it to mainly to help others. It’s more so to help other Veterans in the future, while tracking your own progress as time goes on. One of the best things about it is you’ve got great folks doing phenomenal research. There are a lot of ways to mitigate the problem over time. This program will help with that.”
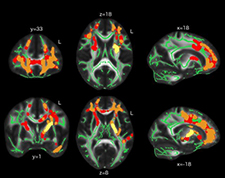
Brain scans that were part of a 2015 TRACTS study documented that blast exposure may lead to change in brain structure even in the absence of outward concussion symptoms.
VA researchers have used data from the TRACTS long-term cohort study to produce more than 100 published papers on traumatic brain injury (TBI) and its accompanying conditions and potential treatments. The following selected studies illustrate the breadth of the rich TRACTS dataset:
--- Mike Richman
VA Research Currents archives || Sign up for VA Research updates