Office of Research & Development |
 |


According to past VA research, a majority of caregivers of service members and Veterans with traumatic brain injury and polytrauma are parents. (Photo for illustrative purposes only. ©iStock/filipefrazao)
August 29, 2018
By Mike Richman
VA Research Communications
The majority of military personnel and Veterans who have served in Iraq and Afghanistan are reporting that they have little trouble readjusting to a normal lifestyle after returning home.
Many others, however, are coming back with serious physical or mental health problems. A large percentage of them are under the age of 30, are unmarried, and are battling traumatic brain injuries, PTSD, depression, or musculoskeletal injuries.
Who cares for these people if they’re unable to function on their own? It’s usually parents who take on that demanding job.
VA researchers hoping to improve the experience of parent caregivers are carrying out a study that compares the effectiveness of two programs. One is called Resources for Enhancing All Caregivers’ Health in the VA (REACH VA), a well-established behavioral program for caregivers. It involves one-on-one telephone sessions focusing on education, support, and skill-building, which are all critical elements for successful caregiver programs. The skill-building includes tips on communication, stress management, problem solving, and reframing negative thoughts.
The other program—or the control group—is based on a recorded webinar presentation. The webinar focuses on caregiving risk factors, such as safety concerns, emotional and physical well-being, and social support. It doesn’t include the skill-building or cognitive reframing components.
"These obligations can lead to parents having to quit their jobs."
The researchers are recruiting 80 parent caregivers to participate in each program.
The goal of the study is two-fold: to determine which program is more effective at helping the parents improve their feelings of depression, anxiety, and burden, and to determine the feasibility of using one-on-one sessions with this population of caregivers.
Dr. Linda Nichols and Dr. Jennifer Martindale-Adams of the Memphis VA Medical Center are leading the three-year trial. They are co-directors of VA’s National Caregiver Center. Staff there are trained to work with caregivers, provide services to caregivers of Veterans and to Vets who are caregivers, and to conduct research on the best practices to help caregivers. Nichols and Martindale-Adams are also on the faculty in preventative medicine at the University of Tennessee.
VA’s Caregiver Support Program funds the National Caregiver Center.
Martindale-Adams says this is the first study to test the effectiveness of a program focusing on parent caregivers of Veterans and service members. Several observational studies have highlighted the challenges faced by that cohort.
“A few years ago, a friend who was an Air Force National Guard general asked us if we’d consider doing the same kind of support work we were doing with caregivers of parents suffering from dementia,” Martindale-Adams says. “So we began working with spouses of post-deployed service members and Veterans struggling with reintegration. Many of those spouses are caregivers, but they don’t always realize it. When we were working with spouses, we got calls from parents asking to be included in our three-year trial because there was nothing there for them. That was the impetus for this study.”

VA center training the next generation of researchers in blood clots and inflammation
Injectable gel could help treat degenerative back pain
VA's new "burden-free" study method finds two blood pressure drugs equally effective
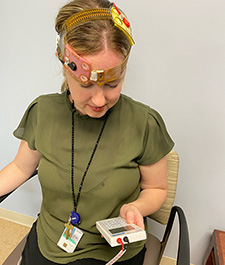
At-home brain stimulation and talk therapy show promise treating chronic pain and PTSD
According to Nichols, increased depression and financial burden are two of the biggest potential consequences for parents taking care of wounded Veterans or service members. Half of caregivers living with people who have suffered multiple traumatic injuries spend at least 80 hours per week helping with such activities as preparing food, getting in and out of bed and the bathroom, and moving around the house. Nearly a third of caregivers of those with less serious injuries spend more than 20 hours a week providing assistance.
“These obligations can lead to parents having to quit their jobs,” Nichols says. “With the financial obligations, parents can wind up dipping into savings and retirement funds.”
She explains that parent caregivers of Veterans and service members face challenges that spouses don’t.
“Although VA’s Program of Comprehensive Assistance for Family Caregivers is a huge resource for parent caregivers and many are served by it, parents don’t have the same access and rights as spouses,” she says. “They cannot manage their adult child’s money unless they seek court approval or become a VA fiduciary, and they may not be able to obtain information on what the child’s medical needs are. Once the children are 18, they are adults.”
She adds: “This is particularly difficult for parents whose children have PTSD. People with PTSD may be distrustful and may not want their parents managing their money. Clinicians aren’t required to tell the parents anything.”
This potential scenario can apply to all parent caregivers, not just those of Veterans and active-duty personnel, according to Nichols.
To be enrolled in the study, which is funded by the Department of Defense, the parents must be caring for a Veteran, a service member, or someone in the National Guard or reserves. They must also report experiencing at least two caregiving stress behaviors, such as feeling overwhelmed, experiencing crying spells or feeling like you need to cry, being frustrated as a result of caregiving, and feeling cut off from family and friends.
The 160 enrollees are being randomized evenly into the REACH VA arm and the webinar arm. Once parents complete the webinar sessions, they are eligible to participate in REACH VA, which started in 2010 as an educational resource for caregivers of Veterans with dementia. It’s run by the National Caregiver Center at the Memphis VA.
In the study, the parents in REACH VA receive six telephone sessions in which coaches in the program give one-on-one instruction in problem solving, how to reframe one’s thoughts, and stress reduction techniques in situations, for instance, involving irritable outbursts by Veterans with PTSD. The sessions are tailored to the needs of the parent.
The parents receive a caregiver notebook to use during the telephone sessions that includes 33 chapters with strategies to handle risk areas. The chapters include tips on overcoming depression, solving problems, and reducing sleep troubles, in addition to suggestions on how to ask for help.
One of the parents in the study is Maxine Christensen, a caregiver for her son Shawn, a 49-year-old Army Veteran (see sidebar). He suffers from nerve and joint damage in his back that he suffered while serving in the military. The back pain has caused him to experience anger and depression issues.
Through REACH VA, Maxine Christensen has learned to walk away from situations when tensions are escalating.
“Once, Shawn was ballistic about some stuff, and I sat here calmly and listened,” she says. “Normally, I’d try to give him an answer or try to get him to settle down. But I didn’t do that for the first time in six years. I was thinking, `How am I feeling right now?’ And my feeling was he is so out of tune that I don’t need to give him an answer. I don’t have an answer. That’s an answer he’s going to have to come up with by himself. He just walked out of the room. He wasn’t mad. He wasn’t upset. He didn’t say anything else. He just went about his business. That’s a change we really needed.”
One way she has learned to back away, Shawn says, is by letting him handle potentially unsettling scenarios with neighbors, such as when they let their dogs do their business in his yard.
“Before, she would intervene and try to defuse the situation,” he says. “It doesn’t really work. To me, it almost feels like I’m being emasculated. But she’s learning that I’m the homeowner, so I’m the one who needs to deal with the situation.”
Before taking part in REACH VA, Maxine completed the webinar sessions, in which the parents are getting some guidance but not the direction that is most critical. The sessions focus on post-9-11 concerns, such as Veteran reintegration, PTSD, traumatic brain injury, and spinal cord injuries, as well as problem behaviors, caregiver health and emotional well-being. The parents are also taught about signs of substance abuse, depression, and possible suicide.
“We could have had a complete control group, in which the caregivers get nothing,” Nichols says. “But that’s hard to do and feels wrong when people are in such need.”
The webinar program, Christensen says, helped her to see what she was doing to herself amid the frustrations of taking care of her son.
“My whole thrust for the first two or three years was all about helping him, fixing this, or finding some way to deal with how he felt,” she says. “I guess that’s what moms do. But it wasn’t working. So by taking part in the webinar sessions, I started looking at what I can do to help myself and channel my emotions the right way.”
No preliminary results from the trial are yet available. The researchers are assessing parent opinions at baseline, at the end of the REACH VA and webinar sessions (both are three months long), and three months after that. Nichols, Martindale-Adams, and their team believe the parents in both groups will improve in the core variables of depression, anxiety, and burden. But they predict the REACH VA program will outperform the webinar program overall.
Meanwhile, Nichols and Martindale-Adams are leading other projects related to caregivers.
They are in the final stages of a study on caregivers of Veterans with multiple sclerosis, a central nervous system disease that disrupts information flow within the brain. They are also partnering with the VA Boston Health Care System on a proposed study of caregivers of Veterans with ALS, or amyotrophic lateral sclerosis, a neurodegenerative disease that affects nerve cells in the brain and the spinal cord.
Plus, they are considering studies on caregivers of Vets with PTSD and dementia, and on the effectiveness of a texting program that could apply to all caregivers. The caregivers would get daily educational text messages from the National Caregiver Center, with the option to receive more information if desired.
“A few months ago, we tested the texting program with caregivers of cancer patients,” Martindale-Adams says. “They were all spouses, siblings, or friends. They loved it.”

Shawn Christensen, who has been coping with chronic pain triggered by a bad fall he incurred during his Army service, has relied on his mother, Maxine Christensen, for caregiving help in recent years. (Photo by Amil Daniels)
For three decades, Maxine Christensen counseled Native Americans on the use of drugs and alcohol. She met with people who abused or were addicted to marijuana, cocaine, heroin, or liquor.
She always felt confident in her ability to connect with those in need of help.
Her command of the situation hasn’t been the same in the seven years she’s been a caretaker for her son, Shawn. He has chronic back pain stemming from nerve and joint damage that resulted from a bad fall he took while carrying heavy equipment at Fort Hood, an Army base in Texas. The back pain has triggered periods of depression and anger that have left her grasping for solutions.
The two live alone in a house that he owns in Ankeny, Iowa. She’s 77 years old, and he’s 49.
“The hard part for me is that I was a counselor for 30 years,” she says. “That was my profession. Not to be able to handle this has been just unbelievable for me. I couldn’t read my son. I probably thought I could say certain things that a counselor would say, not realizing that I needed to separate the two.”
Shawn says living with his mother has required him to make huge sacrifices, including adjusting to the fact that he doesn’t have the same freedom in a household. He’d lived on his own from 1988 when he was 19 and enlisted in the Marines, pretty much until he and his mom began living together in 2011.
“The first couple of years, it took a lot out of both of us in trying to understand how to make this work,” he says. “We’ve learned to agree to disagree on certain issues.”
One of those issues relates to how they handle uncomfortable situations.
“We have differences in mood,” he says. “If I have a bad day, that’s hard on her because if something is wrong, I want it fixed to make it right. My way of fixing it, and her way of fixing it are different. She’s not a really big confrontation person, but confrontation doesn’t bother me at all.”
Maxine says Shawn shows signs of irritability that didn’t exist before his back injury. He’s been diagnosed with a minor form of PTSD.
“It’s so heartbreaking to me to hear my son, the son that I raised, use the foulest language to people on the phone when things aren’t working and not going the way he thinks they should,” Maxine says. “That has gotten worse over the years. I told him one day, `Shawn, I don’t know how much more of this I can really handle because it hurts my heart.’ There’s nothing I can do about it except close the door, leave the house, go out into the yard for a little bit, water the flowers, and not let it get into my head.”
She adds: “We had a discussion the other day, and I said to him, `I think I have the right to say I don’t like that. I don’t think you should talk like that.’ But I don’t really have that right when he’s 49 years old. At the same time, I have felt completely disrespected, and I’ve never felt like that in my life. I never saw my son do that.”
Shawn admits that his mother didn’t teach him to use that language. But it’s something he seems to instinctively do at times.
“Because of my back pain, my anger level can go from zero to 10 non-stop, and I do have an issue with using bad language,” he says. “I don’t think anything of it. If I get in a disagreement with somebody, that can happen. I’ve talked to people on the phone that way when they’re not doing what they should be doing, whether it’s a creditor of whether it’s somebody calling and trying to scam me. It’s hard for her to hear.”
Maxine has learned that the life of a parent caregiver is different than that of a spouse who is caring for a loved one.
“You cannot argue with your child the way that you do what you have to do, stand up for yourself, or work it out if it were a husband and wife situation,” she says. “This is a mom and a son. It’s not the same. That’s a lot of what has been hard for me. I’ve never been an argumentative person or a person that got mad easily.”
In her pursuit of answers, Maxine Christensen has been participating in the randomized trial on parent caregiving being led by Dr. Linda Nichols and Dr. Jennifer Martindale-Adams of the Memphis VA Medical Center (see main article). She has also been in the caregiver support program at the VA Central Iowa Health Care System in Des Moines.
Plus, she’s a member of Blue Star Mothers of America, a group that supports mothers who take part in activities that help service members and Veterans.
Caring for Shawn consumes six to eight hours of her day. She prepares all of his meals and cleans the house mostly on her own. He can’t push a vacuum and is unable to reach down to clean his tub, she says, noting that she’s fine with handling those chores.
Shawn’s therapy, which includes ablations and cortisone shots, relieves some of his pain for a few months before it returns. Maxine reinjured her back during her first year of helping Shawn and has also pursued therapeutic relief.
“We had to sit down and talk about how we’re going to live together at this age,” she says. “We’ve divided responsibilities according to what will work best for him. This isn’t something we ever expected to be doing, especially with the issues that he has. The first area of concern has always been his depression and anger, whichever one comes first. The other issue has been the back pain. One precipitates the other. When his back is better, he deals with life better. The pain doesn’t go away, but he’s amiable. He enjoys life a little bit more. He doesn’t get as upset so quickly. But once it starts wearing off, we go back.”
--- Mike Richman
VA Research Currents archives || Sign up for VA Research updates