Office of Research & Development |
 |

 Shame, one of the emotions associated with PTSD, may have an especially strong role in generating suicidal feelings, research suggests. (Photo for illustrative purposes only. ©iStock/PeopleImages)
Shame, one of the emotions associated with PTSD, may have an especially strong role in generating suicidal feelings, research suggests. (Photo for illustrative purposes only. ©iStock/PeopleImages)
June 10, 2019
By Mike Richman
VA Research Communications
"What surprised us was just how important shame appeared to be."
In the Veteran community, PTSD is often associated with combat trauma. Witnessing a horrific event like a deadly roadside bombing or the killing of a child can take an emotional toll on someone, causing that person to relive the event and feel angry, depressed, or distant.
Does shame—in which a person feels responsible for what happened and views himself or herself as a bad person—play a role in worsening the emotional and day-to-day struggles of someone with PTSD? Shame is a common symptom for those with PTSD.
VA researchers are exploring that question. Some are finding that feelings of shame exacerbate conditions for Veterans with PTSD, even causing them to have thoughts of suicide—what is known as suicidal ideation.
A study led by Dr. Katherine Cunningham, a research psychologist at the Durham VA Health Care System in North Carolina, found that shame “fully accounted for the effects of PTSD on suicidal ideation.” The finding suggests that “shame may represent a key link between PTSD and suicidal ideation among Veterans,” the researchers write.
The study appeared in the Journal of Affective Disorders in January 2019. It included 201 mostly male Veterans who had been treated for PTSD.
Another published paper connected shame to a rise in verbal aggression among Vets with PTSD. Dr. Laura Crocker, a clinical psychologist at the VA San Diego Healthcare System, led the study, which included 127 mostly male Veterans. It appeared in 2016 in the journal Psychological Trauma: Theory, Research, Practice, and Policy.
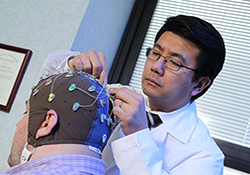
Brain's 'error messages' may hold key to PTSD resiliency

Study explores reasons why Veterans seek—or don't seek—PTSD care
Study: 9 in 10 users happy with PTSD Coach smartphone app
Common peptide may hold key to who gets PTSD, who doesn't
Both studies included Veterans who had experienced combat trauma in the wars in Iraq and Afghanistan. In each paper, the researchers measured the Veterans’ level of shame using the Internalized Shame Scale, which evaluates the extent to which shame becomes magnified and internalized. The scale looks at feelings of inferiority, worthlessness, inadequacy, and alienation in assessing a person’s degree of shame.
Cunningham and her colleagues expected that shame would partly, but not completely, explain why PTSD increases suicidal ideation. They were surprised to learn that shame appeared to be the main reason why PTSD was elevating thoughts of dying by suicide.
“What surprised us was just how important shame appeared to be,” Cunningham says. “Among the Veterans in our study, shame fully explained why PTSD was increasing suicidal ideation. So it was shame and not the other PTSD symptoms that were leading to more suicidal thoughts among the Veterans. This means that shame is an important suicide risk factor that we need to better understand, both for people with PTSD and for those who don’t have PTSD but who do feel intense shame.”
Cunningham says more research is needed to clearly understand why shame is so integral to generating thoughts of suicide.
“Shame appears to play a role for everyone who feels it,” she says. “Why was it so important for these particular Veterans? The honest answer is that we don’t know, and we need to keep doing research to be able to answer that question. In our discussion, we mentioned other things we would want to explore, including whether moral injury may be involved or if era-of-service makes a difference. There are likely certain experiences, such as killing in combat or experiencing other moral injuries, that can increase the likelihood of someone feeling shame and having suicidal thoughts.”
Shame is considered an important element of moral injury, which is essentially a conflict with one’s personal code of morality. For instance, a Veteran may feel guilt, shame, or self-condemnation for violating his or her moral beliefs in combat by killing someone, witnessing death, or failing to prevent the immoral acts of others.
Unlike PTSD, moral injury isn’t a mental health condition. But the symptoms—depression, anxiety, withdrawal, relationship problems, and an increased risk of suicide, to name a few—are similar. Plus, many studies have shown that moral injury and PTSD are related.
In Cunningham’s view, shame and guilt are considered core emotions when someone is experiencing moral injury. “In this respect, shame can be a big part of moral injury, but it’s not the same thing as moral injury,” she says. In 2013, shame and guilt, along with fear, horror, and anger, were included in the diagnostic criteria for PTSD, which is published by the American Psychiatric Association. Although one doesn’t have to carry any of those five trauma-related emotions to be diagnosed with PTSD, patients with the disorder often experience at least one of them.
Research has also shown that PTSD greatly increases someone’s risk for suicidal ideation, but findings are mixed as to whether PTSD elevates risk of death from suicide.
Suicide prevention is VA’s top clinical priority. According to a VA National Suicide Data Report for the period of 2005 to 2015, an average of 20.6 Veterans, including 3.8 active-duty service members, killed themselves each day in 2015. Male Veterans were 1.3 times more likely than non-Veteran adult men to die by suicide in 2015, and female Vets were twice as likely as non-Veteran adult women to kill themselves that year, the report said.
Laura Crocker’s study tested the belief that when shame and guilt are examined together, trait shame, but not trauma-related guilt, would impact the relationship between PTSD symptoms and verbal and physical aggression. This would relate to Veterans seeking treatment for PTSD after experiencing military trauma.
“Trait shame” refers to the idea that some people are more prone to feelings of shame in certain situations, while “state shame” involves feelings of shame in the moment or that day. Trauma-related guilt relates to feelings of guilt about something one did or didn’t do regarding a traumatic event, such as a combat medic feeling guilty about saving one person but not another. Shame and trauma-related guilt are prevalent among combat Veterans.
The researchers found that trait shame partially accounted for the effects of PTSD on verbal aggression but not physical aggression. Crocker and her team were surprised to not find the same impact on physical aggression.
“However, participants in the study reported engaging in physical aggression less often than verbal aggression, which may have made it harder to detect relationships with physical aggression,” Crocker says. “It’s possible that we would observe the expected relationships in people who engage in physically aggressive behavior more often than those in the sample we studied. We also wondered if the participants were less likely to report engaging in physical aggression because of the stigma about the use of violence when one goes to a VA clinic for care. Some other studies have shown links between PTSD, shame, and physical aggression in the context of intimate relationships. So it may also be the case that the context of physical aggression matters.”
In the study, Crocker and her team felt it was important to examine shame and guilt together to see if shame versus guilt played a key role in the link between PTSD and aggression. She explains that shame and guilt are related emotions that overlap a bit, although there’s an important distinction. Guilt is focused on doing a bad thing, while shame equates with feeling like a bad person, she says.
To determine the Veterans’ level of guilt, the researchers used the Trauma-Related Guilt Inventory, a 32-item scale that measures a series of factors. They include the belief that one’s thoughts, feelings, or actions have violated that person’s standards of behavior, such as thinking you’re responsible for the event, and the negative feelings and physical reactions associated with trauma memories.
Interestingly, although the Veterans’ PTSD symptoms were associated with higher scores on all aspects of trauma-related guilt, guilt didn’t significantly impact relations between PTSD symptoms and verbal or physical aggression when accounting for shame.
“Although we found that greater PTSD symptoms were associated with both guilt and shame, the interesting finding was that shame contributes to the link between PTSD and verbal aggression,” Crocker says. “In other words, the higher or more severe one’s PTSD symptoms are, the more likely that person is to experience feelings of shame. In turn, the more likely he or she is to engage in verbal aggression. This was unique to shame. We didn’t find that guilt contributed to the link between PTSD and verbal aggression.”
Crocker and Cunningham believe if someone is diagnosed with PTSD, it doesn’t necessarily mean that person will report feelings of shame.
“Shame definitely can be a symptom of PTSD, but it isn’t always present,” Cunningham says. “And shame, even trauma-related shame, can be felt by people who don’t have PTSD. PTSD usually involves intense uncomfortable emotions, but what people experience varies widely. Someone with PTSD may struggle with fear or anger but not shame. And someone who has experienced trauma may not have PTSD but can still experience shame that leads to suicidal ideation.”
Both researchers have been studying shame in the context of PTSD for several years. Cunningham’s interest in the subject stemmed from her research on Veterans whose PTSD symptoms didn’t seem to dissipate, even though they were working hard in treatment. They shared in common “very deep-seated, incredibly painful beliefs about themselves that they were now broken or horrible people because of traumas they had experienced,” she says. These beliefs led to intense feelings of shame, she notes.
“For example,” she says, “a theme that I heard a lot is combat stories involving the deaths of children. If Veterans are or believe they are responsible for a child dying, they may begin to believe that they are a bad person, thinking `what kind of person would hurt a child.’ These beliefs can be reinforced by other people, such as when Vietnam Veterans were called `baby killers’ after they returned home.
“Negative beliefs about ourselves are intensely emotional,” she adds. “For most people, that means we don’t question those thoughts. We just accept them as true. In a way, the intense emotion that we feel serves as `proof’ for the underlying thought, for example, `I feel guilty so I must have done something wrong.’ And because it hurts so much, we naturally want to avoid feeling it and thinking about what caused it. We also want to hide it from other people, because we don’t want them to think the same things we do about ourselves. But when we hide what’s hurting us, we don’t get the chance to process it and maybe learn something new, like, `I’ve done things I regret, but I’ve done good things too. I’m still a good person, and people like me.’ If we get a better understanding of how shame and shame-related thoughts play a role in PTSD and affect suicide risk among Veterans, then we have the opportunity to better help Veterans live the lives they want when they return home.”
Crocker agrees that shame in the context of PTSD needs to be better understood.
“There has been some important work studying shame in people with PTSD and trying to understand the links between shame and PTSD,” Crocker says. “However, more work is certainly needed to better understand what leads some people to experience shame more than others, how shame is related to various negative outcomes, such as mental health symptoms, substance abuse, aggression, and suicidality, and how to best treat shame in order to reduce the negative consequences of it.”
Crocker notes that a co-author of her 2016 study, Dr. Sonya Norman of VA San Diego, is currently leading research to examine Trauma Informed Guilt Reduction Therapy (TrIGR), a cognitive-behavioral psychotherapy that is designed to treat guilt and shame resulting from trauma and moral injury. The therapy can be administered in at least four 60- to 90-minute sessions and includes three major elements:
Norman is also the director of the PTSD Consultation Program at VA’s National Center for PTSD, which offers consultation, continuing education, and other resources to medical providers who treat Veterans with PTSD. A 2014 pilot study led by Norman suggested that TrIGR may help reduce the severity of trauma-related guilt and associated distress.
“We need to better understand shame both in the research community and in our clinical work,” Cunningham says. “If we understand shame better and can get better at treating it, that has implications for lowering suicide risk and improving mental health treatment, not just for PTSD but for other mental health issues, as well. This is especially important for our ability to help Veterans, because they face a host of suicide risk factors, including PTSD and moral injury.”
VA Research Currents archives || Sign up for VA Research updates